Waardenburg syndrome (WS) is a rare condition that affects the facial bone structure, as well as hair, skin, and eye pigmentation. First described by geneticist Petrus Johannes Waardenburg in 1951, Waardenburg syndrome is inherited in an autosomal dominant manner (passed from a parent with a mutated gene to a child).1 One mutated gene is enough to cause the condition.
This article reviews Waardenburg’s syndrome and its symptoms, causes, specific ocular manifestations, potential impacts, and current treatment options.
How Does Waardenburg Syndrome Affect Eye Health?
Waardenburg syndrome affects eye health due to its impact on eye color. According to Dr. Brian P. Brooks of the National Eye Institute (NEI), “The less melanin is present, the worse vision tends to be.”8
The melanin density in your eyes determines how dark your eyes appear and how best they can tolerate bright light and ultraviolet (UV) radiation from the sun.9 The darker your eyes are (due to more melanin), the less the visual discomfort in bright, sunny conditions or when driving at night.
People with Waardenburg syndrome have a low concentration of melanin pigment, characterized by very pale blue eyes or different-colored eyes (partial albinism). It makes them prone to the following vision issues:
- UV damage
- Cataracts
- Macular degeneration
- Sensitivity to light (photophobia)
- Reduced visual acuity (low vision)
- Strabismus (Misalignment of the eyes)
- Iris transillumination (light entering the eye through the iris instead of the pupil)
- Monocular vision (seeing with one eye)
Can Waardenburg Syndrome Cause Blindness?
Although rare, the ocular consequences of Waardenburg syndrome may be severe enough to cause blindness. For example, a lack of melanin in the eye causes the accumulation of free radicals in the eye’s retina.10 These elements play a role in age-related macular degeneration (AMD). AMD causes gradual loss of central vision and is a leading cause of blindness among older people.
Partial albinism in the eye also allows ultraviolet (UV) radiation from the sun to damage all eye structures, including the eye lens. The lens may become cloudy, causing reduced vision (cataracts).11 Continuous deterioration of the eye lens can eventually cause blindness.
What is Waardenburg Syndrome?
Waardenburg Syndrome (also Waardenburg’s) is a rare genetic disorder. It’s characterized by:
- Hearing loss
- Unusual bone structure
- Discolored hair, skin, and eyes
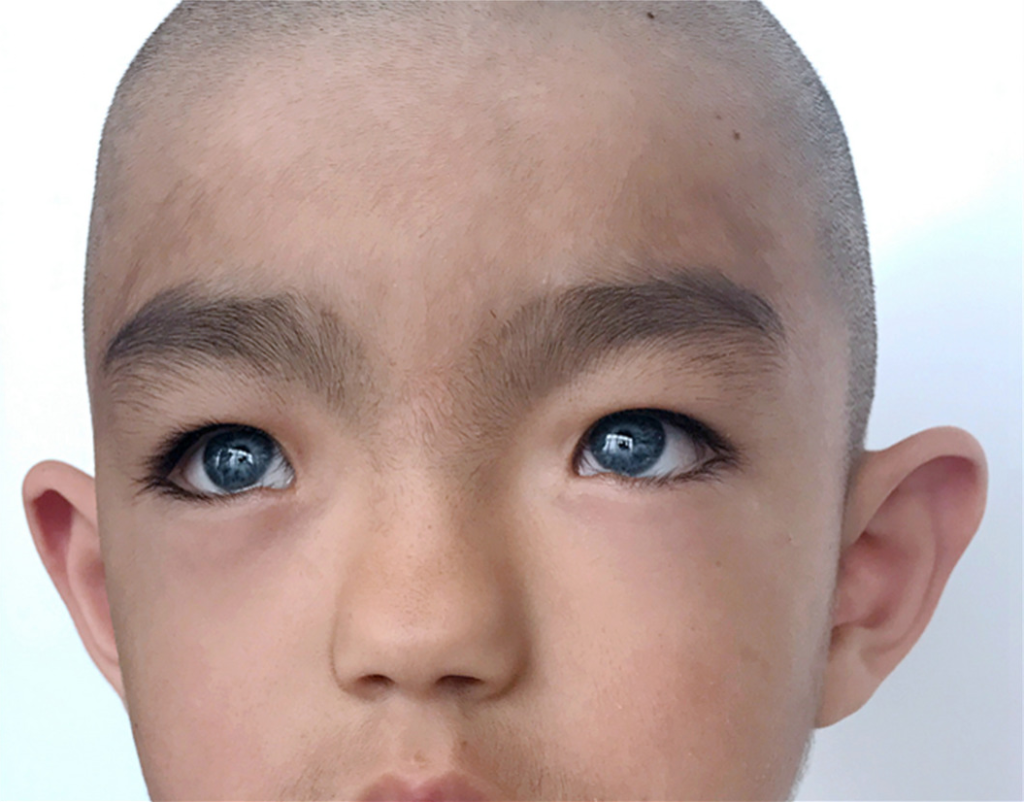
Waardenburg syndrome may also cause hearing loss and digestion issues. This condition may affect more than one family member, but the symptoms can differ from person to person.
According to researchers, Waardenburg syndrome affects 1 in 40,000 people.3 This condition also accounts for 2 to 5% of all cases of deaf newborns (congenital hearing loss).
Factors Causing Waardenburg Syndrome
Most people with Waardenburg syndrome have at least one parent with the illness. However, in isolated cases, mutations may cause Waardenburg syndrome in people with no family history.
Advanced paternal age (father's age) is considered one factor influencing new mutations. It may cause Waardenburg syndrome and other dominantly inherited disorders among people with no family history.2
Types of Waardenburg Syndrome
There are four types of Waardenburg syndrome:
- Type I. Causes hearing loss, a wide space between the eyes (orbital hypertelorism), broad nasal root, and synophrys (meeting eyebrows). It may also cause abnormal hair, iris, and skin pigmentation.
- Type II. Similar to type 1 but with a higher possibility of hearing loss (50%)
- Type III (Klein-Waardenburg syndrome). Causes all Type I and Type II symptoms, including arm, hand, or shoulder abnormalities.4
- Type IV (Waardenburg-Shah syndrome). Includes symptoms of Waardenburg syndrome (Type I, II, and III) and Hirschsprung disease.5 Hirschsprung disease is an intestinal disorder responsible for severe constipation or blockage of the digestive tract.
Types I and II are the most common forms of Waardenburg syndrome.
What Causes Waardenburg Syndrome?
Waardenburg syndrome comes from mutations (variations) in several genes involved in forming special cells, including melanocytes (pigment-forming cells). The lack of melanocytes producing melanin, which causes hair, skin, and eye pigmentation (coloring), leads to abnormal pigmentation.
Melanin also plays a significant role in the normal function of the inner ear. According to research, a lack of melanin in the inner ear increases the risk of noise damage and causes poor sound localization in space.6
The following six genes undergo mutations causing Waardenburg syndrome:
- EDN3. Causes Waardenburg syndrome Type IV due to its function in the formation of intestine nerves (enteric nerves).
- EDNRB. Causes Waardenburg syndrome Type IV due to its function in the formation of intestine nerves (enteric nerves).
- MITF. Causes Waardenburg syndrome Type II.
- PAX3. Causes Waardenburg syndrome Types I and III.
- SNAI2. Causes Waardenburg syndrome Type II.
- SOX10. Causes Waardenburg syndrome Type IV.
What are the Symptoms of Waardenburg Syndrome?
Symptoms of Waardenburg syndrome vary depending on the type of Waardenburg syndrome you have. WS Type III (Klein Waardenburg syndrome) tends to be the most debilitating.
Common symptoms of WS include:
- Constipation when combined with Hirschsprung disease (WS Type IV)
- Moderate to severe hearing loss (common in WS Type II)
- Pale blue eyes or eye colors that don’t match (heterochromia)
- Difficulty completely straightening joints
- Pale skin, hair, and eyes
- Dystopia canthorum or widely spaced eyes (WS Type I and II)
- White patch on hair or early graying of the hair
- Meeting eyebrows (synophrys)
- Finger bones fused together (WS Type III)
- Abnormalities of the upper limbs and intestinal blockage (WS Type IV)
- Microcephaly or an unusually small head (WS Type III)
- Cleft lip (rare)
People with Waardenburg syndrome may develop self-esteem issues and other problems related to their appearance. Studies also show a possibility of slight intellectual decline (mental impairment).7
Visit your doctor if you experience severe symptoms that affect your quality of life, such as hearing loss or frequent constipation.
Listen In Q&A Format
How Does Waardenburg Syndrome Affect Eye Health?
Vision Center Podcast
Does Waardenburg Syndrome Affect Other Body Parts?
Beyond vision, Waardenburg syndrome can also affect other areas of a person’s life. These include:
- Hearing loss. Waardenburg syndrome causes defects in inner ear structures and accounts for 2 to 5% of all congenital deafness cases.
- Cosmetic changes to eyes, skin, and hair. Differently colored eyes, white patches on the skin, and premature graying of hair affect appearance and influence self-esteem.
- Intellectual disability. Although research on this is limited, scientists believe that congenital deafness could affect a person’s ability to develop intellectually.
- Bowel problems. In some cases, Waardenburg syndrome co-occurs with Hirschsprung disease, causing constipation or intestinal blockages. This is common in Waardenburg syndrome Type IV.
- Unusual facial bone structure. Such as a wide space between the eyes, a broad nose, etc.
- Abnormalities of hands and arms. These may include abnormally short upper limbs, abnormally bent finger joints, fused wrist bones, webbed fingers, or abnormal elevation of the shoulder blades (Sprengel deformity).
A case report in The British Journal of Development Disabilities described a possible link between WS Type III and autistic spectrum disorder, aggressive behavior, and intellectual disability. However, more research is needed to confirm this.13
How is Waardenburg Syndrome Diagnosed?
Waardenburg syndrome can be diagnosed at birth (congenital WS), early childhood, or later in life. Diagnosis will come from clinical evaluation, physical findings, family history, and other specialized studies.
A doctor can diagnose Waardenburg syndrome using major and minor criteria developed by the Waardenburg Consortium.
Minor criteria
- White patches of skin (leukoderma)
- Meeting eyebrows (Synophrys)
- broad nasal bridge
- Underdeveloped nostril
- Premature graying of hair
Major criteria
- Sensorineural deafness
- Dystopia canthorum (widely spaced eyes)
- Abnormal iris pigmentation, such as heterochromia iridis
- Abnormal hair pigmentation, such as a white forelock, discolored eyebrows, or eyelashes (poliosis)
- Family history of Waardenburg syndrome
A positive Type I Waardenburg syndrome diagnosis involves two major or one major and two minor criteria. Type II involves two major criteria, excluding abnormalities of the inner corner of the eye.
Exams and Tests for Waardenburg Syndrome
The following tests and exams are involved in diagnosing Waardenburg syndrome:
- A complete eye exam. It requires a slit-lamp examination to check for vision and eye health.
- Audiometry. It tests a person’s hearing ability.12
- Bowel transit time test. It determines the time it takes for food to travel through the digestive system.
- Colon biopsy. It requires removal and microscopic examination of colon tissues to help confirm Hirschsprung disease.
- Molecular genetic testing (gene sequencing). It requires taking DNA samples to confirm the diagnosis and detect disease-causing mutations.
- Advanced imaging. It involves using imaging technology, such as computed tomography (CT) scanning and X-rays, to visualize inner ear defects that cause congenital deafness.
Note that these tests cannot determine how severe the symptoms of Waardenburg syndrome will be. If your child is diagnosed with Waardenburg syndrome, monitor their developmental milestones to ensure symptoms do not hinder their intellectual development or quality of life.
Treatment for Waardenburg Syndrome
Waardenburg syndrome has no specific treatment method, but affected persons can still live normally. Waardenburg syndrome’s symptoms are usually treated when they arise.
Commonly recommended treatments include the following:
- Special diets and bowel medicines. A diet with high fiber can help with constipation.
- Eye protection such as sunglasses and hats. To prevent the harmful effect of sunlight on the eyes.
- Vision aids. Wearing contact lenses and eyeglasses address low vision associated with partial albinism.
- Cochlear implant surgery. Using implants that are placed behind the ear to manage hearing loss.
- Wearing sunscreen. To protect the affected skin from sun damage.
- Bowel surgery. To remove the affected segment of the colon or repair affected intestines in patients with Hirschsprung syndrome.
- Topical ointments or cosmetics. To help conceal the white skin patches.
- Hair dye. To help cover a white forelock and other unpigmented hairs.
- Cognitive behavioral therapy. To help the affected person build confidence and self-esteem.
- Physical therapy and orthopedic techniques. To treat upper limb abnormalities.
Discuss your treatment options with your doctor to determine what best serves your situation.
Can You Prevent Waardenburg Syndrome?
Since Waardenburg syndrome is a genetic condition, you cannot prevent it. However, parents can get their genes tested to determine the risk of having a child with this genetic disorder.
Outlook and Prognosis
People with Waardenburg syndrome Type I and II can live a normal life once its symptoms are addressed. However, those with rarer forms of the condition (Type III and IV) may have other complications, such as constipation and physical deformities.
Talk to your doctor if you’re concerned about a family history of Waardenburg syndrome. You may benefit from genetic counseling if you plan to have a family.
Summary
- Waardenburg Syndrome (also known as Waardenburg’s) is a rare genetic disorder characterized by hearing loss, unusual bone structure, and discolored skin, eyes, and hair.
- According to researchers, Waardenburg syndrome affects 1 in 40,000 people and accounts for 2 to 5% of all cases of congenital hearing loss.
- There are four types of Waardenburg syndrome: Type I, Type II, Type III, and Type IV. Type I and Type II are the most common.
- Mutations in the following six genes form the basis for Waardenburg syndrome: EDN3, EDNRB, MITF, PAX3, SNAI2, and SOX10.
- Waardenburg syndrome can be diagnosed at birth, early childhood, or later in life. Diagnosis is based on clinical evaluation, physical findings, family history, etc.
- There is no treatment for WS, but symptoms can be managed. Common treatments include eyeglasses or contact wear, skin treatments, hair dyes, ear implants, and more.
- You may benefit from genetic counseling if you’re concerned about genetic mutations causing Waardenburg syndrome.
- More research is needed to increase knowledge and develop better treatment strategies for Waardenburg syndrome.



