Glaucoma affects about 3 million Americans and is the second leading cause of blindness worldwide.1 There are many types of glaucoma varying in symptoms and severity, all involving optic nerve damage.
Glaucoma is diagnosed during a routine comprehensive eye exam by a licensed ophthalmologist. Early detection is the key to stopping glaucoma, so undergoing regular eye exams is critical.
In this article, we cover the different types of glaucoma, its potential causes, and potential treatment options.
What Is Glaucoma?
Glaucoma is an umbrella term for eye conditions that damage the optic nerve, the crucial link between the eye and the brain. It is caused by increased intraocular pressure (IOP), which eventually damages the optic nerve.
IOP happens when there's a buildup of aqueous humor, the fluid that flows throughout the front part of your eye.
Normally, aqueous humor flows through the pupil to the front of the eye. Then, it drains through channels between your iris and cornea, called the drainage angle. Eye pressure can increase if the fluid balance is off slightly, causing glaucoma.

5 Types of Glaucoma
The most common types of glaucoma stem from problems with the eye’s drainage angle. However, other types of glaucoma can result from a different health condition or injury that causes an increase in IOP.
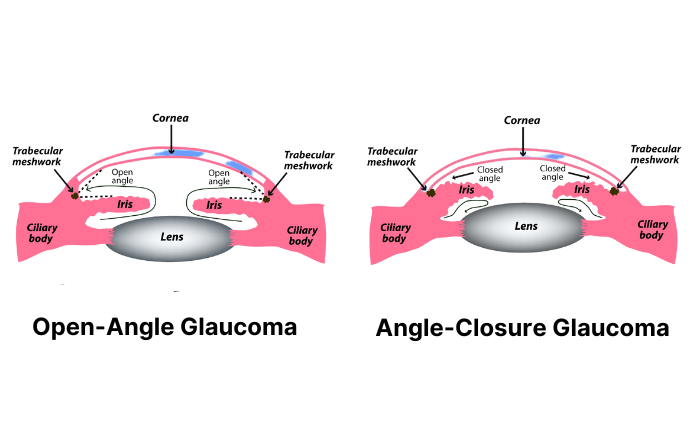
1. Acute Angle-Closure Glaucoma
Acute angle-closure glaucoma is an uncommon type of glaucoma caused by the iris slipping into a position that blocks the drainage angle. The blockage increases eye pressure rapidly, causing an acute attack. It's also referred to as closed-angle glaucoma or narrow-angle glaucoma.
Acute angle-closure glaucoma is considered a medical eye emergency. It requires immediate treatment from an ophthalmologist to prevent permanent vision loss or blindness.
Symptoms
Acute angle-closure glaucoma is considered acute because the IOP rises faster. Warning signs are usually noticeable right away and include:
- Hazy or blurred vision
- Severe pain in the eye or forehead
- Eye redness
- Rainbows or halos
- Headache
- Nausea
- Vomiting
If you have any of these symptoms, seek medical treatment right away. A delay in treatment could result in blindness.
2. Open-Angle Glaucoma
Open-angle glaucoma is the most common type of glaucoma. Open-angle means that access to the drainage angle is open.
Open-angle glaucoma is often associated with a gradual progression of increased IOP. It's often caused by a slowing drainage rate, similar to a clogged drain.
Symptoms
Since it happens over time, there is typically no pain or symptoms to warn you of the increased IOP and damage to the optic nerve. The absence of symptoms can lead to a late diagnosis when vision loss has already started.
The first warning signs of open-angle glaucoma are typically blind spots in your peripheral vision (side vision). Other symptoms may include:
- Use of stairs becomes difficult
- Eye ache
- Cloudy vision
3. Secondary Glaucoma
Secondary glaucoma occurs due to a secondary medical issue that increases eye pressure. This includes conditions like eye injury, inflammation, diabetes, etc.
Secondary glaucoma is either an open-angle or angle-closure type and may occur in one or both eyes. Common types of secondary glaucoma include:
- Steroid-induced glaucoma. Stems from steroid eye drops or systemic steroid use
- Trauma-induced glaucoma. A condition typically caused by blunt-force trauma
- Uveitic glaucoma. Causes inflammation in the middle layer of the eye
- Neovascular glaucoma. Occurs when newly formed blood vessels cover the drainage angle. It’s typically associated with diabetes
- Exfoliative glaucoma. Caused by a flaky material falling off the eye lens, clogging the drainage angle
- Pigmentary glaucoma. Develops from pigment dispersion syndrome when pigment material breaks free and clogs your drainage angle
Symptoms
Depending on the underlying cause of secondary glaucoma, there may not be any symptoms until vision changes appear. Like open-angle glaucoma, symptoms usually begin with blind spots in peripheral vision.
4. Normal-Tension Glaucoma
Normal-tension glaucoma is a damaged optic nerve not caused by increased eye pressure. It's also called low-tension glaucoma and normal-pressure glaucoma.
People diagnosed with this type of glaucoma have normal eye pressure. It’s currently considered a form of open-angle glaucoma.
Symptoms
Because normal-tension glaucoma is a type of open-angle glaucoma, there are usually no signs or symptoms until the optic nerve damage progresses into vision loss.
5. Pediatric Glaucoma
Congenital glaucoma, also called pediatric or childhood glaucoma, is a rare condition that occurs when a baby’s drainage canal does not develop properly in vitro. It’s typically diagnosed within the first year of life and is often hereditary.
Symptoms
Symptoms of congenital glaucoma typically include:
- Enlarged eyes
- Cloudiness
- Excessive tearing
- Sensitivity to light
Who Is at Risk of Developing Glaucoma?
Certain medical conditions and lifestyle factors can contribute to elevated eye pressure, increasing the risk of developing glaucoma. These risk factors include:
Family History of Glaucoma
You'll likely develop the condition if your parents, grandparents, siblings, or other close relatives have glaucoma. According to the Glaucoma Research Foundation, family history increases the risk of glaucoma four to nine times.11
African-American, Asian, and Hispanic Populations
Certain ethnic backgrounds are at higher risk than Caucasians to develop glaucoma. One survey found that, in the US, glaucoma is six times more prevalent in individuals of African descent than in the European American (EA) population. This difference in glaucoma prevalence is only observed in some age groups.12
History of Steroid Use
Steroid-induced iatrogenic glaucoma was first described in the 1950s. One study shows that long-term corticosteroid use can cause an elevation in eye pressure.13
Eye Injury
Trauma to the eye is also a risk factor for glaucoma. This is also called traumatic glaucoma.
A significant blow to the eye—such as in a car accident— can cause an elevation in eye pressure, which may lead to glaucoma if left untreated.
Other Risk Factors
Other risk factors of glaucoma include the following:
- Being over the age of 55
- Severe myopia (nearsightedness)
- Hypertension (high blood pressure)
- Thinner cornea (less than .5 mm)
When to See an Eye Doctor for Glaucoma
Routine comprehensive eye exams are critical in maintaining eye health and catching early warning signs. It’s essential to see an eye doctor if you notice any vision changes, including:
- Blurry or double-vision
- Dark spots
- Sensitivity to light
- Changes to your peripheral vision (side vision)
- Eye pain or frequent headaches

You should also get an annual eye exam if you're over 35 and have a high risk for glaucoma.
When Is Glaucoma A Medical Emergency?
Seek care right away if you experience:
- Sudden loss of vision in one or both eyes
- Sudden blurry, hazy, or double vision
- Flashes of light
- Dark spots in your side or central vision
- Halos or rainbows around light
- Severe eye pain
Listen In Q&A Format
Glaucoma: Types, Symptoms, Causes, and Treatment
Vision Center Podcast
How Is Glaucoma Diagnosed?
Glaucoma is diagnosed during a comprehensive eye exam by a licensed ophthalmologist. The exam consists of tests to check the eyes' overall health.
Many exams dilate the pupils, which allows the eye doctor to look at the retina, optic nerve, and the back of the eye. Tonometry is another critical eye test that measures intraocular pressure in both eyes.
Other tests used to diagnose glaucoma include:
- Visual acuity test (distance and clarity)
- Visual field test
- Measure corneal thickness
- Look at the drainage angle
Treatment Options for Glaucoma
There’s no cure for glaucoma, and optic nerve damage is irreversible. However, many glaucoma treatments can help slow the progression of the disease and minimize vision loss.
Medication
The first goal of treatment is to reduce IOP to prevent further optic nerve damage. Lowering IOP is done by using prescription eye drops, which must be administered for the rest of your life.
Various types of medicated eye drops are available, including:
- Beta-blockers. Helps reduce the amount of fluid in the eye, lowering the pressure
- Alpha-adrenergic agonists. Increases outflow and minimizes the production of eye fluid
- Carbonic anhydrase inhibitors. Reduces eye fluid production
- Miotic or cholinergic agents prostaglandins. Helps increase eye fluid outflow
- Prostaglandin. Helps increase eye fluid outflow
Laser Surgery
Laser therapy treats glaucoma when medications alone no longer lower eye pressure. It aims to repair and unblock the drainage angle.
Types of laser therapy used to treat glaucoma include:
- Trabeculoplasty. A procedure that opens clogged channels in the drainage angle
- Iridotomy. A surgical procedure that creates a small hole in the iris (colored part of the eye) to drain eye fluid
Glaucoma Surgery
Glaucoma surgery is necessary when medication and laser treatment no longer reduce eye pressure.
The type of surgery needed depends on the drainage system issue. Options include:
- Trabeculectomy (filtering surgery). Opens the sclera (white part of the eye) and removes part of the trabecular meshwork to help eye fluid drain freely
- Drainage implant. Involves placing a tube on the sclera to help fluid drain out of the eye and reduce eye pressure
- Cataract surgery. Involves replacing the lens (helps focus light on the retina) and can promote eye pressure reduction for people with narrow-angle glaucoma
Can You Prevent Glaucoma?
While glaucoma can’t be cured or prevented, there are lifestyle changes that can help slow disease progression, including:
- Annual comprehensive eye exams
- Exercise
- A healthy diet
- Not smoking
- Eye protection
- Blood sugar and pressure control
Summary
Glaucoma is an umbrella term for eye diseases that damage the optic nerve. The condition is caused by increased intraocular pressure (IOP). It results in vision loss and eventual blindness if not treated early.
Glaucoma is typically asymptomatic until the advanced stages of the disease. The first warning sign of glaucoma is changes in peripheral vision (side vision).
Early detection is vital to minimize vision loss and prevent blindness. Glaucoma is diagnosed during an annual comprehensive eye exam. These exams are recommended for anyone experiencing symptoms or with a high risk of developing glaucoma.



