If you’re considering LASIK, this page should be your starting point.
Use it to understand the basics first, then branch into the pages that matter most for your decision: cost, candidacy, safety, recovery, and LASIK alternatives such as PRK or lens replacement.
Start Here
- Trying to decide if LASIK is worth it? Read this guide first, then compare LASIK cost and LASIK safety.
- Wondering if you qualify? Review the candidacy section below, then read LASIK and age and LASIK recovery time.
- Comparing procedures? Also read PRK, SMILE, and lens replacement.
- Trying to estimate savings? Use the LASIK cost calculator.
This guide covers what LASIK is, what to expect before, during, and after surgery, and the key tradeoffs to understand before you book a consultation.
What is LASIK Eye Surgery?
LASIK stands for laser-assisted in-situ keratomileusis. It’s a type of refractive eye surgery that involves using a laser beam to correct vision problems caused by refractive errors.
The refractive errors this surgery can treat include:
- Myopia (nearsightedness)
- Hyperopia (farsightedness)
- Astigmatism (an imperfection in the corneal curvature)
How Does LASIK Work?
LASIK surgery involves reshaping the corneal tissue using a laser device. This corrects the way light focuses on the retina.
The procedure typically involves two key laser technologies:
- Femtosecond laser. This laser is often used first to create a corneal flap, which is then gently lifted.
- Excimer laser. With the flap lifted, the excimer laser reshapes the underlying corneal tissue according to your eye's unique prescription, correcting how light focuses on the retina.
What are the Benefits of LASIK?
LASIK offers the potential for long-term vision correction, particularly for moderate myopia (nearsightedness), with a low chance of vision regression over time.
It’s a relatively painless procedure, with most people experiencing significant vision improvements the next day.
While temporary dry eye is common post-surgery, the risk of developing chronic dry eye is relatively low. Additionally, there’s no need for bandages after the procedure. LASIK also has an impressive success rate of over 90%.
Additionally, LASIK is cost-effective compared to the cumulative expense of glasses and contact lenses. But for most people, LASIK is a great way to enjoy life without contacts or glasses.
What is the Satisfaction Rate of LASIK Eye Surgery?
More than 95% of LASIK patients achieve at least 20/25 unaided vision, with over 90% achieving the coveted 20/20 or better outcome.
The outcome provides long-term stability. Over 90% of patients remain glasses-free after a decade.
Because of this, the satisfaction rate of LASIK is very high. 95 to 99% of LASIK recipients would choose the procedure again or recommend it.
What Are the Risks of LASIK?
The most common post-operative side effect is temporary dry eye. Around half of the patients experience mild dryness, halos, and glare immediately after surgery.
By six months, about 20% – 40% of patients still report dry-eye symptoms, and persistent dryness is seen in roughly 10% – 30% of cases.
Flap complications are also uncommon, especially with femtosecond lasers. These potential complications include:
- Flap dislocation. Occurs in roughly 0.003% of femtosecond cases, significantly lower than the 0.03% with microkeratome-created flaps.
- Epithelial ingrowth. Cells invading beneath the flap are rare (<1%) and typically easily managed if detected early.
The most serious complication of LASIK eye surgery is corneal ectasia. This is a serious complication, involving progressive corneal thinning.
Does LASIK Need Touch-Ups?
Sometimes, LASIK might not achieve the full desired correction (under-correction) or, rarely, go slightly beyond the target (over-correction). Vision may also subtly change or regress over time for a small percentage of patients.
To address this, surgeons may perform a LASIK enhancement. It’s easy and quick, as it only involves re-lifting the initial flap for further correction.
Many LASIK packages include no-cost enhancements within the first year. Be sure to verify your surgeon’s enhancement policy upfront to avoid unexpected costs later.
What to Expect During the Procedure
The surgeon will apply some numbing eye drops before placing a small suction ring to stabilize your eye, preventing movement.
A corneal flap is then made using a femtosecond laser or microkeratome blade. An excimer laser then reshapes the cornea by carefully removing microscopic layers, correcting refractive errors.
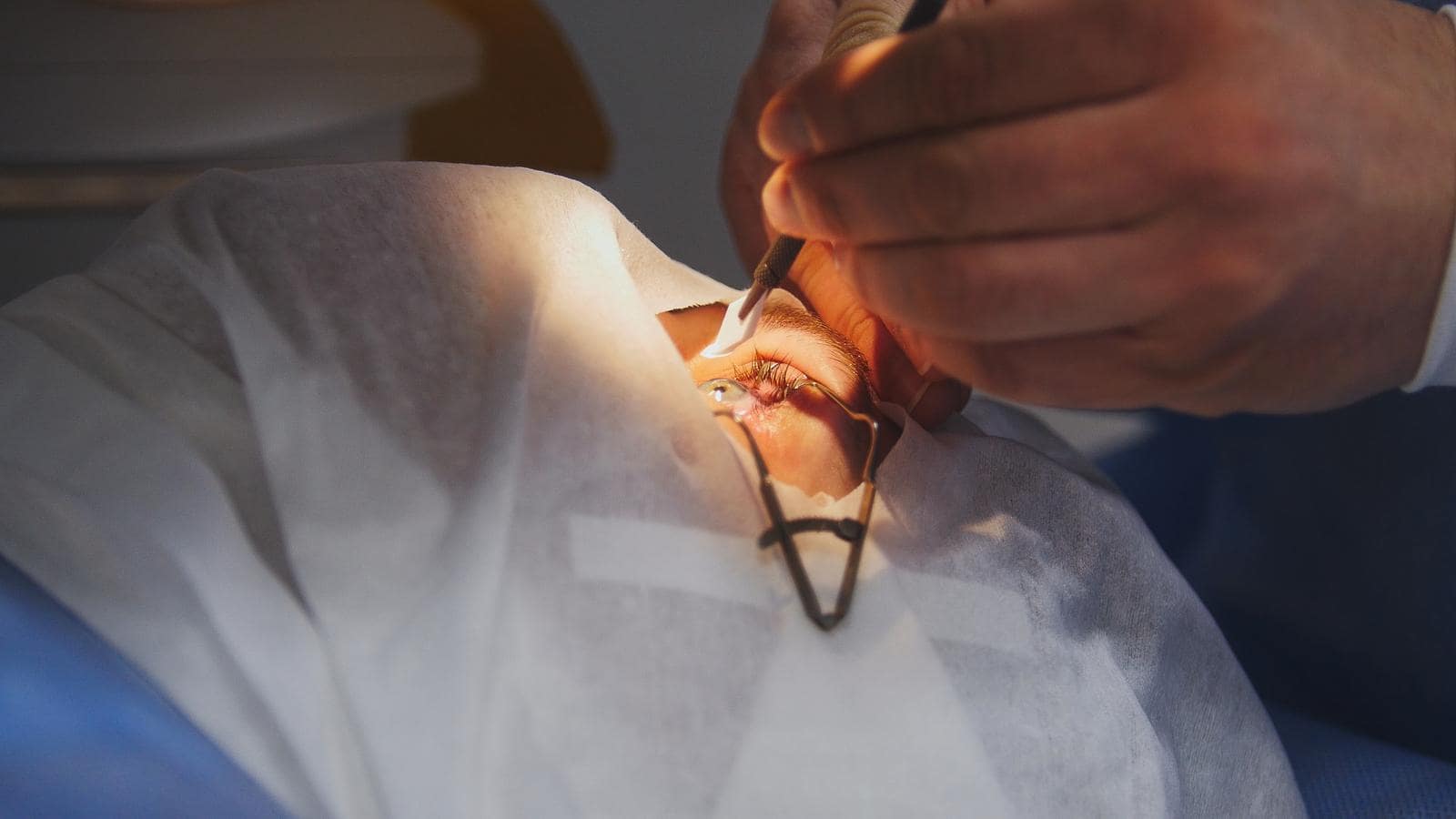
The entire LASIK procedure typically lasts about 10 minutes per eye, and you'll spend approximately an hour at the surgical center from start to finish.
What Happens After the Procedure?
The surgeon smoothly replaces the flap, which naturally adheres without stitches. Many notice significantly improved vision soon after the procedure, sometimes even immediately.
After surgery, your doctor will provide you with post-op care instructions:
- Resting with your eyes closed or sleeping for a few hours can help manage initial discomfort as the numbing drops wear off.
- Wear an eye shield to avoid accidentally touching or injuring your eye.
- Take a few days off work, especially if your job requires intense eye use.
- Use prescribed antibiotic eye drops and ointments provided by your doctor.
What to Avoid After Laser Eye Surgery
Avoid the following during recovery:
- Rubbing your eyes
- Swimming and hot tubs (for about a week)
- High-impact activities and contact sports
- Eye-straining activities such as excessive reading
Continuous monitoring of the healing process is very important. You should make your first follow-up appointment at least 24 hours after surgery and plan regular visits.
Who is a Good Candidate for LASIK?
Not everyone is a candidate for laser eye surgery. Your doctor will ensure you meet specific requirements before recommending LASIK as a vision correction option.
You’re a good candidate for LASIK if:
- You’re 18 years or older, though many surgeons prefer patients to be in their mid-20s when vision prescriptions tend to be more stable.
- Your refractive error falls between roughly -1 and -12 diopters for nearsightedness, or up to +6 diopters for farsightedness.
- Your corneas meet minimum thickness criteria, ensuring sufficient structural integrity remains after surgery.
- You have a refractive error (myopia, hyperopia, or astigmatism).
- You have a stable vision prescription (at least 1 to 2 years) to reduce the chances of regression.
- You have ideal corneal thickness (this reduces the chances of corneal ectasia).
- You want to reduce or eliminate dependence on glasses or contact lenses.
- Set realistic expectations.
Who Isn’t a Good Candidate for LASIK?
Reasons that may disqualify a patient from LASIK include:
- Pregnancy or nursing
- Thin corneas or signs of keratoconus (corneal bulging, often identified through advanced corneal mapping techniques)
- Underlying health issues, such as immunodeficiency or autoimmune diseases
- Presence of cataracts (cloudy eye lens)
- Severe dry eye, previous eye injury or surgery, and eye conditions
- Taking certain medications that can impair healing, such as systemic immunosuppressants or some high-dose anti-inflammatory drugs (discuss all medications with your surgeon)
- Your lifestyle includes high-risk activities such as contact sports, which increase the risk of flap complications
How Much Does LASIK Cost?
The cost of LASIK in the U.S. averages around $4,400 for both eyes, typically ranging between $2,200 and $3,000 per eye.
Because it’s considered an elective surgery, most insurance plans don’t cover the cost of LASIK. Check your insurance plan to see if it provides coverage or benefits for refractive surgery like LASIK.
Fortunately, many surgical practices offer financing plans to help reduce the cost of LASIK. You can also use a flexible spending account (FSA) or a health savings account (HSA) to reduce the overall cost of the procedure.
Find an Eye Doctor Near You
Ready to explore if LASIK is right for you? The first step is a comprehensive eye exam and consultation with a qualified ophthalmologist.
Use VisionCenter’s ‘Find an Eye Doctor’ tool to locate qualified specialists nearby. For additional expert guidelines, visit resources provided by reputable organizations like the American Academy of Ophthalmology (AAO) or the American Optometric Association (AOA).



