Updated on February 20, 2024
Iritis: Symptoms, Causes & Treatments


Vision Center is funded by our readers. We may earn commissions if you purchase something via one of our links.
What is Iritis?
Iritis is inflammation of the iris, the colored ring of muscle fibers around your eye’s pupil. Another name for iritis is anterior uveitis. It’s the most common type of uveitis.
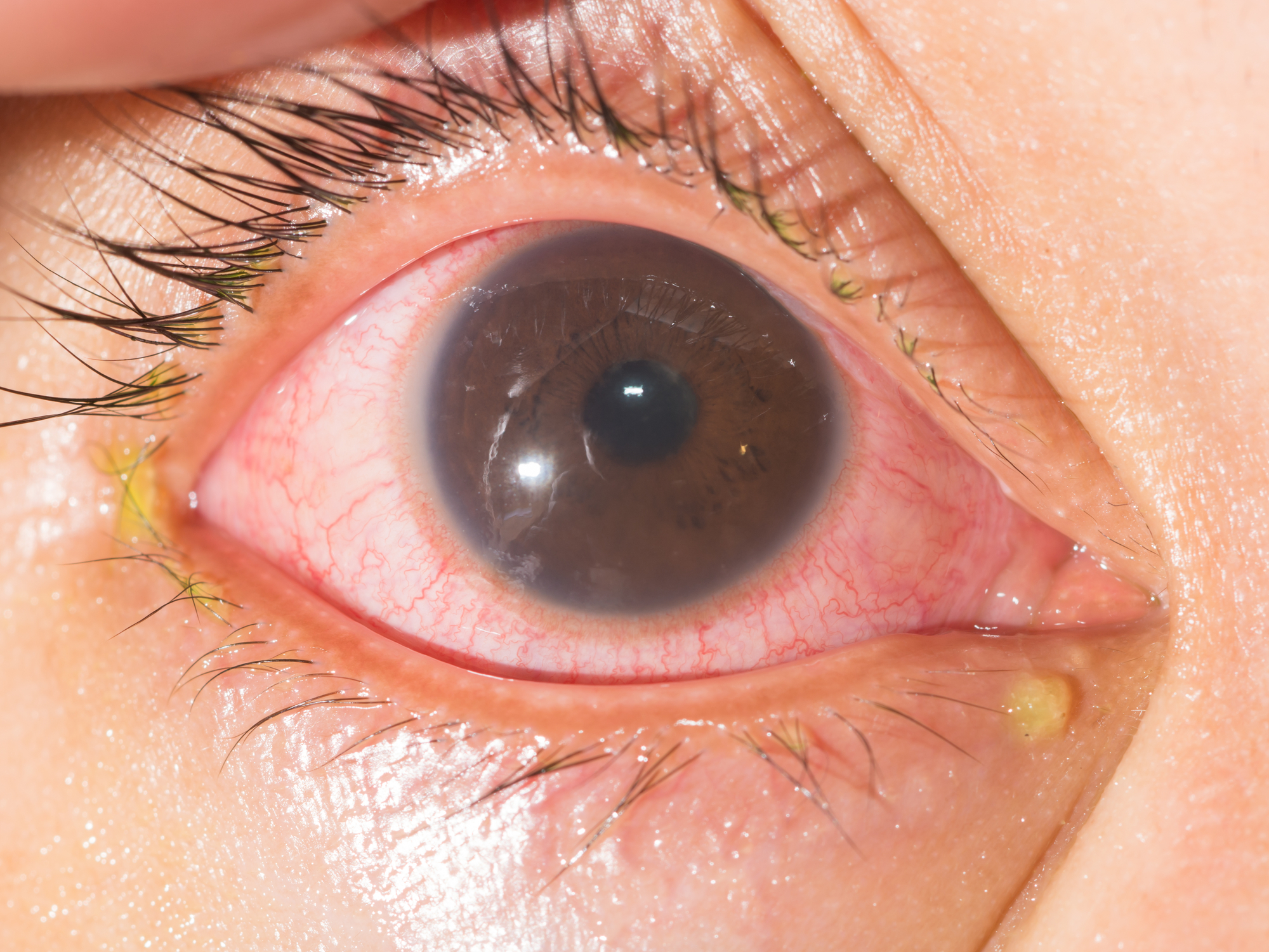
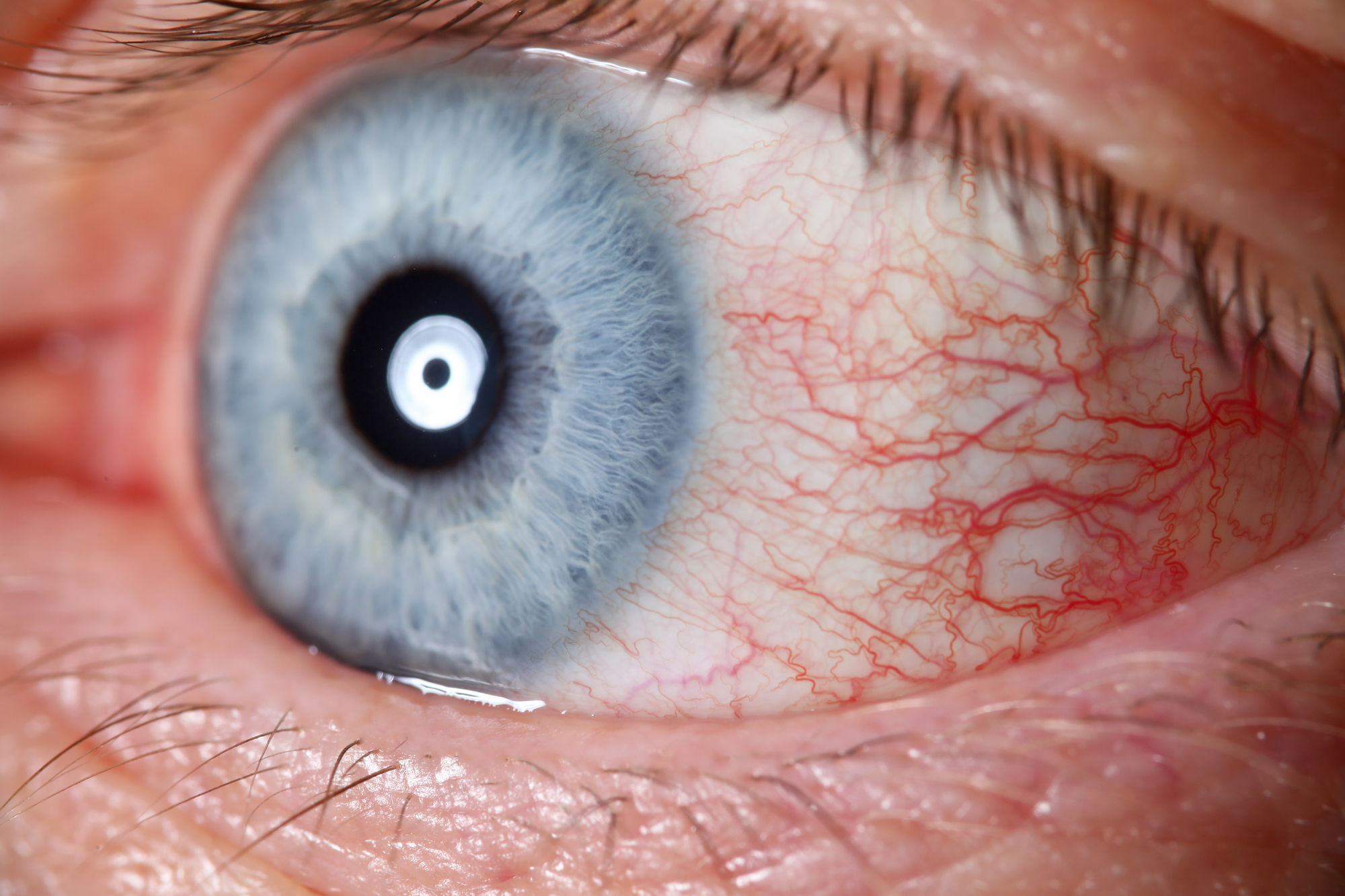
Uveitis is an inflammatory eye disease that affects any part of the uvea. The uvea is the middle layer of your eye, located between the white of the eye (sclera) and the retina. The iris is the front (anterior) part of the uvea.
What are the Symptoms of Iritis?
Iritis symptoms usually develop suddenly and can affect one or both eyes. See your healthcare provider at the earliest signs of iritis.
Signs and symptoms include:
- Eye pain
- Blurry vision
- Eye Redness
- Sensitivity to bright light
- Decreased vision
- Headache
- An increase in floaters
- An unusually small or misshapen pupil
Acute iritis develops over hours or days. When symptoms develop gradually or last longer than three months, it’s considered chronic iritis.
Is Iritis Serious?
Untreated iritis and uveitis can lead to serious problems, including glaucoma or severe vision loss.
Prompt medical attention can reduce the risk of complications from iritis. Call your doctor at the first sign of symptoms.
When to See a Doctor for Iritis
Seek medical care as soon as possible if you have symptoms like eye pain or blurred vision. Prompt treatment can prevent serious complications from developing.
In addition to seeing your eye care provider, scheduling a consultation with your primary care physician is a good idea. They can determine whether an underlying inflammatory disease or infection is causing your iritis.
What Causes Iritis?
Most of the time, the cause of iritis is unknown. It can be linked to various health conditions, genetic factors, and eye trauma.
Causes of iritis include:
Injury
Acute iritis can be caused by an eye injury. Common examples include:
- Blunt force trauma
- Burns from chemicals or a fire
- An object that punctures the eye
Infections
Iritis can result from several types of infections, including:
- Viral infections on your face. Such as cold sores and shingles.
- Bacterial infections. Including tuberculosis, Lyme disease, and syphilis.
- Other infectious diseases. These include parasites like toxoplasmosis and fungus such as histoplasmosis.
Autoimmune Diseases
People with certain autoimmune disorders due to genetic factors that alter their immune function may also develop acute iritis.
The most common conditions include:
- Ankylosing spondylitis (a type of arthritis)
- Reactive arthritis
- Psoriatic arthritis
- Lupus
- Rheumatoid arthritis
- Inflammatory bowel diseases like ulcerative colitis
Juvenile Rheumatoid Arthritis
Also known as juvenile idiopathic arthritis, this is the most common form of arthritis that affects children. Chronic iritis can occur in children with juvenile rheumatoid arthritis.
Sarcoidosis
This autoimmune disease involves the development of tiny collections of inflammatory cells called granulomas. It usually affects the lungs and lymph nodes but can occur in any part of the body, including the eyes.
Certain Medications
Some drug therapies for conditions like HIV and osteoporosis can be a rare cause of iritis. These medications include:
- Rifabutin (Mycobutin)
- Cidofovir
- Bisphosphonates
Who is at Risk of Developing Iritis?
Anyone can develop iritis, but some people have a higher risk.
Risk factors for non-traumatic iritis include:
- Genetic predisposition to autoimmune diseases
- Sexually transmitted infections (STIs) such as syphilis and HIV/AIDS
- Having a weakened immune system or an autoimmune disorder
- Smoking tobacco
Traumatic iritis can happen to anyone. This is one of the reasons it’s so important to protect your eyes when engaging in activities that put your vision at risk.
What are the Potential Complications?
Iritis can lead to dangerous complications if left untreated. Potential complications associated with untreated iritis include:
- Cataract formation. Clouding of the lens of the eye.
- Irregular pupils. Scar tissue can affect the shape and function of the pupil.
- Glaucoma. Recurrent iritis can lead to a serious eye condition that involves increased eye pressure.
- Deposits on the cornea. This leads to degeneration of the cornea and decreased vision.
- Cystoid macular edema. Fluid-filled cysts and swelling in the retina can blur or reduce central vision.
How is Iritis Diagnosed?
To diagnose iritis, your eye doctor will perform a comprehensive eye exam. This includes:
- External exam. Using a penlight, your doctor will check your pupils for redness and signs of discharge.
- Visual acuity. This checks the sharpness of your vision using an eye chart.
- Slit-lamp exam. Your doctor will use a lighted microscope to view the inside of your eye and look for signs of iritis.
Additional tests, such as blood tests and X-rays, may be necessary to determine the underlying cause of iritis.
Iritis Treatment
Iritis treatment aims to relieve pain and inflammation and prevent permanent vision problems. If an underlying health problem causes iritis, that condition must also be treated.
Treatment typically includes:
- Topical steroid eye drops. To reduce inflammation.
- Dilating eye drops. To reduce pain and prevent further complications.
- Oral medications. These include steroids or other anti-inflammatories if eye drops do not alleviate symptoms.
Severe or recurring cases of iritis and complications may require surgical treatment.
Outlook
Professional diagnosis and treatment of iritis are necessary to prevent serious complications. Effective treatment reduces discomfort, as well as the risk of secondary problems.
Iritis caused by trauma usually clears up within a couple of weeks. Non-traumatic iritis can take weeks or months to heal.
If the cause of iritis is a bacterial or viral infection, the condition will go away after you treat the infection.
People with chronic iritis associated with systemic diseases might be able to treat iritis at home based on their doctor’s recommendations. Your ophthalmologist may provide you with steroid eye drops to have on hand when symptoms flare up.
Tips for Managing Iritis at Home
You can do several things at home to manage iritis symptoms until you can get medical attention.
For example:
- Apply a warm compress. For 20 minutes three to four times a day.
- Wear glasses with dark lenses with UVA and UVB protection. To ease light sensitivity and pain.
- Use eye drops recommended by your doctor. As directed and never touch the tip of the bottle to your eyes.
Summary
Iritis is the most common form of uveitis, an inflammatory eye condition. Signs and symptoms of iritis involve eye pain, redness, and blurry vision.
Seek medical care as soon as possible if you have iritis symptoms. Left untreated, it can cause severe and permanent vision loss. Treatment with topical steroids is usually effective.
Iritis may be associated with injuries, infections, and autoimmune conditions. Often, the exact cause is unknown.
In this article
5 sources cited
Updated on February 20, 2024
Updated on February 20, 2024
About Our Contributors
Kelly Brown, a content writer for Vision Center, is dedicated to sharing vital information to assist individuals in making informed decisions about their vision health. Her writing covers a range of topics, from selecting the best eye doctor to addressing health issues impacting vision, with the aim of educating readers through informative and engaging content.
Dr. Melody Huang is an optometrist and freelance health writer with a passion for educating people about eye health. With her unique blend of clinical expertise and writing skills, Dr. Huang seeks to guide individuals towards healthier and happier lives. Her interests extend to Eastern medicine and integrative healthcare approaches. Outside of work, she enjoys exploring new skincare products, experimenting with food recipes, and spending time with her adopted cats.

