Defects to any part of your eye may adversely affect your vision and quality of life. One defect of the eye is a macular pucker.
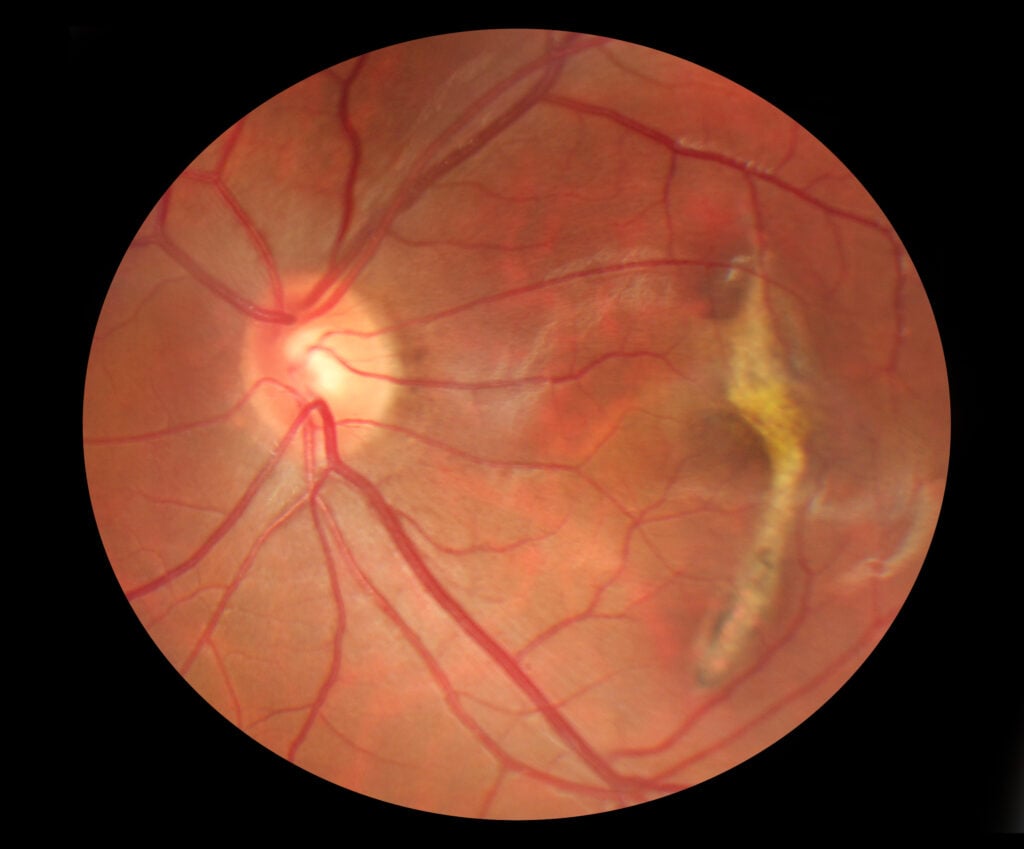
Fundus photo of macular scarring with normal blood vessels and optic nerve
A macular pucker is a scar tissue or wrinkle on the eye’s retina. It affects the eye’s ability to focus clearly on objects.
In this article, we’ll explore this condition and offer insights into the following:
- What a macular pucker is, and what causes it
- Symptoms of a macular pucker
- Diagnosis of a macular pucker
- Available treatments for macular pucker
What Is a Macular Pucker?
A macular pucker, or wrinkled retina, is scar tissue that forms on the macula. The macula is the central area of the retina responsible for detailed vision.1
Other names of macular pucker are:
- Retinal folds
- Cellophane maculopathy
- Epiretinal membrane (ERM)
- Preretinal membrane
- Surface wrinkling retinopathy
- Pre-macular fibrosis
- Epimacular membrane
The retina is the light-sensitive back layer of the eye. It sends visual signals to the brain for interpretation, with its center (macula) being the enabler of detailed vision.
Effect of a Macular Pucker
When scar tissue forms on the macula, the ability of the retina to focus light is impaired, resulting in blurry vision. Your eye won’t be able to focus light properly, even if you wear eyeglasses.
Retinal folds or a wrinkled retina are generally not a serious condition and most people experience only mild vision distortion that may not require any treatment. In rare cases, however, it can result in severe vision loss or lead to a related condition known as a macular hole.
Disability Considerations
According to the Americans with Disabilities (ADA), a disability is any physical or mental impairment that substantially limits one or more major life activities.
A macular pucker isn't considered a disability because it does not completely impair your ability to see. This distinction is important for understanding how macular pucker affects daily life and what legal and social definitions of disability it does not meet.
Symptoms of a Macular Pucker
Most cases of macular pucker have mild symptoms that may get worse with time. Someone with a macular pucker may experience the following:
- Straight lines like electric cables, line grids, or railway lines appear wavy
- Blurry vision
- Difficulty seeing clearly, even with glasses
- Double vision (diplopia)
- Images seen by the affected eye may appear larger (macropsia)
Some people get used to the changes in vision. If you’re concerned or notice any changes in your vision, talk to your eye doctor.
Does Macular Pucker Cause Floaters?
A macular pucker does not cause floaters.5 However, floaters are a good indicator for related causes of macular pucker, such as retinal tear, posterior vitreous detachment, and diabetic retinopathy.
What Causes a Wrinkled Retina?
Most cases of macular puckers are idiopathic.3 This means that there is no known cause. However, scientists agree that aging plays a major role in the wrinkling of the macula.
The vitreous is a clear liquid that fills the eye and gives it a round shape. The vitreous slowly shrinks as you age and pulls away from the retina.
Usually, it pulls away and separates without any problems in a process called posterior vitreous detachment (PVD).4 However, the vitreous may sometimes pull away without detaching, leaving membrane or scar tissue and causing a wrinkled retina.
Who Is at Risk for a Macular Pucker?
Macular puckers are common among people aged 50 or older. The National Institutes of Health reports that 20% of people aged 75 or over have macular puckers.2
However, you can develop a macular pucker at any age. Your risk of macular pucker is higher if you:
- Have small dark spots, threads, or cobwebs floating across your vision (floaters)
- Have a history of vitreous detachment
- Have a history of retinal tear or retinal detachment
- Have a history of uveitis or eye inflammation
- Have retinal blood vessel disorders
- Had eye surgery, including cataract surgery
- Had severe eye injury
A macular pucker usually occurs in one eye, but both can be affected. Most people experience only mild visual distortion that may worsen gradually.
Macular Pucker Diagnosis
Your doctor will check for macular pucker during a dilated eye exam. Your doctor will use dilating eye drops to widen your pupil and examine the inner parts of your eye.
If macular pucker is suspected, they’ll perform other confirmatory tests such as:
- Amsler grid eye test. A page of small squares made of horizontal and vertical lines is used to check whether straight lines appear wavy or distorted.
- Optical coherence tomography (OCT). This test examines the thickness of your macula and detects any swelling or visual distortion. It also assesses treatment effectiveness.6
- Fluorescein Angiography (FA). This test examines retinal blood circulation. Photos of your eyes are taken to check for potential leakage as blood flows through the eye.
Treatment Options for Macular Pucker
Most people with macular puckers have mild symptoms and do not require treatment. However, healthcare professionals encourage regular eye exams to ensure the condition does not worsen.
Your eye doctor may recommend a new eyeglass prescription, reading lamps, and other magnifiers to improve visual acuity. If a macular pucker affects your quality of life by hindering important activities such as reading and driving, your eye doctor may recommend surgery.
Common surgeries for macular pucker include:
- Vitrectomy surgery. An outpatient procedure that involves removing some vitreous gel and peeling off the abnormal membrane from the retina’s surface
- **Membranectomy.**7 Removal of the abnormal membrane from your retina using precision surgical instruments; it doesn’t involve vitreous gel removal
- **Fluidic Internal Limiting Membrane Separation (FILMS).**8 A new procedure still under development; after vitrectomy, a fluid is injected between the membrane and the retina, causing the scar tissue to lift away
Is Surgery Effective for a Macular Pucker?
Surgery will significantly improve your distorted central vision. However, the exact outcome is hard to predict.
Not undergoing the recommended surgical procedure increases your risk of complications such as severe vision loss or macular holes. However, full blindness is impossible since macular puckers only affect central vision and not peripheral vision.
What to Expect After Treatment
After surgery, an eye shield will be placed over your eye for protection. Wear the eye shield for at least the first 24 hours. You’ll also receive eye drops to help reduce inflammation and prevent infection.
Any applied stitches will dissolve within 4 to 6 weeks. Your eyes may feel gritty and appear red while the stitches are present. Full recovery can take about 3 to 6 months.
Post-Surgery Care
To reduce pain and prevent ocular pressure on your treated eye, the American Academy of Ophthalmology (AAO) recommends sleeping face down, with the operated eye hanging off the edge of the bed.9 Do this for a period recommended by your doctor.
You can use special equipment such as face-down pillows, chairs, and mirrors to help you maintain your position. You’ll also be required to moderate certain activities to ensure a successful healing process.
These activities include:
- Driving
- Intense exercise
- Swimming
- Air travel
- Applying make-up
- Rubbing your eyes
If you experience severe pain, worsening vision, or any concerning side effects, consult your doctor for better management.
Summary
- A macular pucker, or wrinkled retina, is scar tissue that forms on the macula, the central area of the retina responsible for detailed vision.
- A macular pucker usually occurs in one eye, but both can be affected. Most victims experience only mild vision distortion that may worsen gradually.
- Common symptoms of macular pucker include blurry vision, floaters, double vision, etc. Frequent eye exams can help monitor any worsening symptoms.
- Most cases of macular pucker do not require treatment. In severe cases, eye doctors recommend surgery to restore vision.
- See your doctor's advice if you experience blurry vision or any concerning symptoms.



