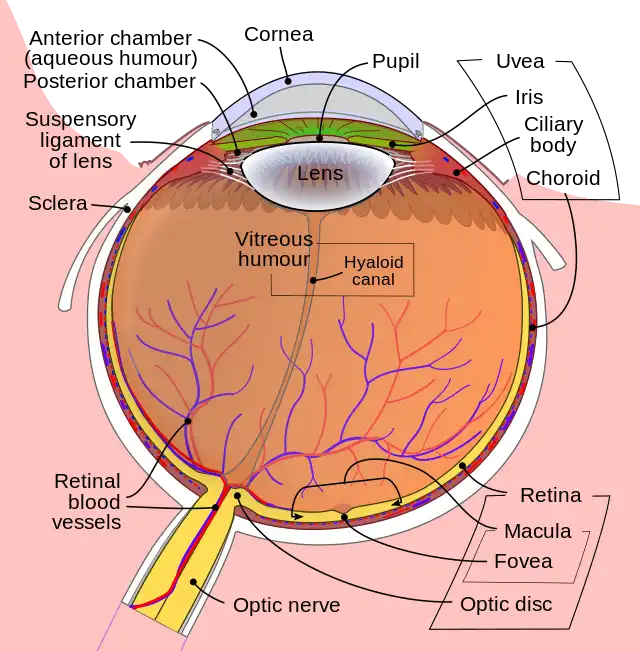
The vitreous humor, also known as the vitreous body or the vitreous, is a clear, gel-like substance that fills the space between the lens and the retina in the eye.
This transparent, colorless fluid makes up about 80% of the eye's volume and plays several crucial roles in maintaining ocular health and function. Its gel-like consistency helps maintain the eye's shape and supports the retina.
The vitreous humor consists of approximately 99% water, with the remaining 1% composed of:
- Collagen fibers
- Hyaluronic acid
- Proteins
- Salts
- Sugar
In this article, we’ll discuss practical tips for supporting the health of your vitreous humor and maintaining optimal eye health. You’ll also learn how the vitreous humor contributes to vision, the common conditions affecting it, and the available treatment options.
How Does the Vitreous Humor Contribute to Sight?
The vitreous humor plays a critical role in vision by contributing to several essential functions within the eye. Here’s how it contributes to the visual process:
- Structural support. It helps maintain the eye's shape and keeps the retina in place against the back of the eye. This is crucial because a detached retina can lead to significant vision loss.
- Light transmission. Its transparent nature allows light to pass through to the retina. The retina is a layer of light-sensitive cells at the back of your eye that converts light into signals your brain interprets as images.
- Shock absorption. The gel-like consistency acts as a cushion, protecting the eye from minor impacts and vibrations.
- Nutrient distribution. Although it doesn’t help provide vision, the vitreous humor transports essential nutrients to the lens and retina, ensuring that they are healthy and functional.
What Conditions Affect the Vitreous Humor?
Several common conditions can affect the vitreous humor, resulting in various visual disturbances or complications. Understanding these conditions is crucial for proper diagnosis and treatment.
Early detection and treatment can help prevent vision loss and other complications associated with these conditions affecting the vitreous humor.
Some of the most common conditions include:
1. Posterior Vitreous Detachment (PVD)
PVD is a common age-related condition where the vitreous humor separates from the retina. It often occurs as the vitreous becomes more liquid-like with age.
Symptoms may include:
- Sudden increase in floaters
- Flashes of light
- Potential risk of retinal tears or detachment
2. Vitreous Hemorrhage
A vitreous hemorrhage occurs when blood leaks into the vitreous humor. It can be caused by diabetic retinopathy, retinal tears or detachment, or eye trauma.
3. Vitreous Degeneration
As people age, the vitreous humor can undergo degenerative changes, including liquefaction (synchysis) or the formation of opacities (syneresis). These changes can lead to an increase in floaters and other visual disturbances.
4. Vitreomacular Traction Syndrome
This condition occurs when the vitreous humor pulls on the macula, potentially causing distorted vision, decreased visual acuity, and macular edema.
Macular edema is a condition where fluid accumulates in the macula, which is the central part of the retina responsible for sharp, detailed vision.
5. Proliferative Vitreoretinopathy (PVR)
PVR is a serious complication that can occur after retinal detachment surgery or severe eye injuries. It involves the growth of scar tissue in the vitreous cavity and on the retina, potentially leading to recurrent retinal detachment.
6. Uveitis
Inflammation of the uvea can affect the vitreous humor, causing:
- Increased protein levels in the vitreous
- Cellular infiltration
- Changes in vitreous transparency
Different types of uveitis, such as chronic uveitis and lens-induced uveitis (LIU), can lead to distinct patterns of inflammatory mediators in the vitreous.
Treatment Options for Vitreous Humor Conditions
Treatment for the aforementioned conditions typically depends on the cause, and in some cases, there are no specific treatments. For example, with vitreous degeneration, the symptoms typically clear off or become less bothersome.
There’s also no specific treatment for PVD. Most people get used to the floaters in their visual field and improve with time. However, some conditions require medical treatment.
Treatment for Retinal Tears and Detachment
If you’re diagnosed with a retinal tear or detachment, your doctor may recommend surgery. Common surgical procedures for retinal tears and detachment include:
- Photocoagulation. Laser beams are used to repair retinal tears.
- Freezing (Cryopexy). A freezing probe is used to create a scar on the retinal tear to secure the retina in position.
- Vitrectomy. Removes the detached retina and replaces the vitreous fluid.
- Scleral buckling. A procedure to correct retinal detachment. Involves placing a band/buckle on the sclera to hold the retina in position.
- Pneumatic retinopexy (PR). Injects air or gas into the vitreous cavity to increase its volume and allow reattachment of the retina to the eyeball.
Treatment for Vitreous Hemorrhage
Most cases of VH do not require treatment as the blood can clear off from the vitreous fluid with time as long as there is no further damage. However, severe cases may necessitate the following procedures:
- Laser photocoagulation. Treats abnormal or leaky blood vessels and repairs retinal damage.
- Anti-VEGF injections. Shrink abnormal blood vessels in the eye.
- Cryotherapy. Use of low temperatures to treat tears and detachments that cause bleeding.
- Vitrectomy. Replacing the bloody vitreous humor with a substitute fluid.
During a dilated eye exam, your eye doctor can check for vitreous abnormalities. If you experience floaters, flashes, vision changes, or severe eye pain, seek immediate medical attention. These may indicate a potential problem.
Tips to Maintain Eye Health in Relation to Vitreous Humor
While the vitreous humor might seem hidden away in your eye, several lifestyle choices and habits can impact its health. Here are our tips to keep your it healthy:
- Eat a balanced diet rich in antioxidants (vitamins C and E, lutein, zeaxanthin), omega-3 fatty acids, and zinc.
- Drink plenty of water to maintain the fluid balance in your eyes, including the vitreous humor.
- Exercise regularly to improve blood circulation, delivering essential nutrients and oxygen to your eyes.
- Quit smoking to reduce the risk of cataracts, macular degeneration, and other eye conditions that can indirectly affect the vitreous humor.
- Wear sunglasses that block 99% to 100% of UVA and UVB rays to protect your eyes from harmful UV rays.
- Manage screen time to prevent digital eye strain, which leads to dry eyes and potentially affects the health of the vitreous humor over time.
Why Should You Get Regular Eye Check-ups?
Regular eye exams are crucial for maintaining healthy vision and detecting potential issues early on. Comprehensive eye exams assess the overall health of your eyes, including the vitreous humor, retina, and optic nerve.
These can detect early signs of conditions like glaucoma, macular degeneration, and retinal detachment, which can indirectly affect the vitreous humor.
Your eye doctor can also provide personalized advice on maintaining eye health and managing any existing conditions.



