What is Polycoria of the Eye?
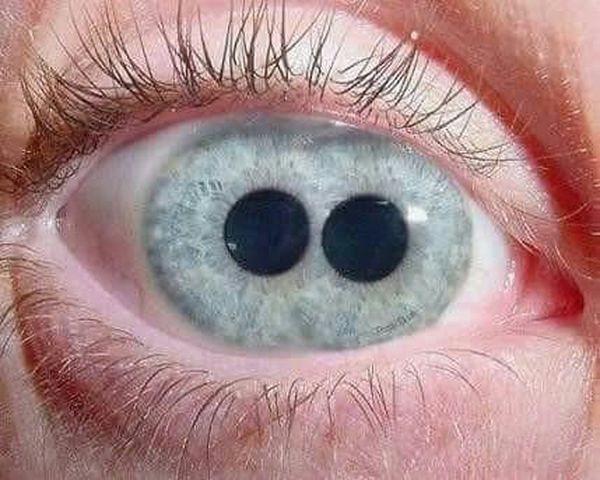
Polycoria is an eye condition affecting the pupils. It is when two pupils are present in one eye.
The condition is typically present in childhood but may not be diagnosed until later in life. Some people experience double vision in the affected eye.
Polycoria can affect either the left eye or right eye. In some cases, it can affect both eyes.
Is Polycoria a Rare Condition?
Polycoria is extremely rare. Other conditions are commonly mistaken for it. There are no known trends in the development or occurrence of polycoria based on geographical location, gender, age, or season.
What Causes Polycoria?
The underlying cause of polycoria is unknown. However, some conditions have been linked with polycoria.
Conditions associated with polycoria include:
- Polar cataracts
- Glaucoma
- Abnormal development of the pupil margins
- Eye development abnormalities
- Poor vision
- Retinal detachment
What are the Signs and Symptoms of Polycoria?
The signs and symptoms of polycoria usually result from having more iris muscles than usual.
The iris is the colored ring of muscle circling each pupil. The iris adjusts how much light reaches the eye.
In polycoria, the pupils are usually smaller than usual and are separated by individual parts of the iris. This can mean that less light enters the eye.
This can dim your vision. You may struggle to focus because the pupils are not working effectively.
The primary symptom of polycoria is the appearance of two pupils.
Other signs and symptoms of polycoria may include:
- Blurred vision in the affected eye
- Poor, dim, or double vision in the affected eye
- An oblong shape of one or all additional pupils
- Issues with glare
- A bridge of iris tissue between the pupils
How Does Polycoria Affect Vision?
The vision complications of polycoria include:
- Blurred vision
- Poor vision
- Vision difficulties from the glare of lights
These vision complications of polycoria result from a less effective iris and pupil.
Types of Polycoria
There are two types of polycoria, including:
True Polycoria
People with true polycoria have two or more separate pupils in one eye.
Each pupil has an intact sphincter muscle that will individually constrict and dilate.
True polycoria is extremely rare. The condition can affect vision. A person with true polycoria also experiences stimulation of the retina in response to bright lights.
The term true polycoria is overused. Sometimes it is used to misdescribe a case of pseudopolycoria.
Pseudopolycoria
Pseudopolycoria is less rare than true polycoria. However, it is still very uncommon.
In cases of pseudopolycoria, there is ‘passive constriction.’ Passive constriction differentiates the additional pupil from the actual pupil during dilation and constriction.
The additional pupil in pseudopolycoria is different from the extra pupil in true polycoria. This is because it displays defects that are independent of the sphincter muscles.
Pseudopolycoria involves splitting the iris that is not due to the sphincter muscles at the root of the iris.
Pseudopolycoria is often linked with the following conditions:
- Seckel syndrome
- Posterior polymorphous dystrophy
- Juvenile glaucoma
Listen In Q&A Format
Polycoria: Two Pupils in One Eye
Vision Center Podcast
Treatment Options for Polycoria
Some people with polycoria do not require any treatment because their vision is not affected.
For anyone whose vision becomes difficult due to polycoria, surgery is one possible treatment option.
However, because true polycoria is rare, it can be challenging to determine the most effective treatments.
Pupilloplasty
One case report has shown that surgery was an effective treatment option.1 This type of surgery is called pupilloplasty.
During pupilloplasty, the surgeon cuts through the iris tissue. This removes the ‘bridge’ that has developed between the two pupils.
During this surgery, the patient is placed under retrobulbar anesthesia, and the pupils are dilated with one percent tropicamide.
The surgery, in this case report, was successful and improved the individual’s vision.
More trials are necessary to determine whether pupilloplasty will be effective for everyone with true polycoria. However, as true polycoria is rare, there have not been enough cases to determine a success rate for this treatment.
Polypropylene Suture
Another surgical procedure used to treat polycoria is the use of a double-armed polypropylene suture. The suture is left externally on the sclera with a knot buried in the scleral flap.
This technique enables posterior fixation of intraocular lens implants in the absence of capsular support.
Polycoria Outlook
The outlook for polycoria is typically good. Patients may not require any treatment if the visual impairment is minimal and does not interfere with daily life.
However, if treatment is necessary, pupilloplasty has so far shown successful results. If you have polycoria, it is essential to receive regular check-ups with an eye doctor to monitor your vision and any adjustments in your eyes.
Having your eyes checked regularly is also advantageous for your eyesight as a whole.
Possible Complications of Untreated Polycoria
There are various complications resulting from untreated polycoria.
These complications include:
- Blurred vision
- Poor vision
- Vision difficulties from the glare of lights
Such complications result from a less effective iris and pupil. Pseudopolycoria, or holes in the iris that appear as extra pupils, can also be part of Axenfeld-Rieger syndrome. This syndrome is a group of eye conditions that can affect eye development.
Should You Be Worried if One Pupil Is Bigger Than the Other?
Approximately 15 to 30 percent of people have different-sized pupils. Usually, this is not dangerous and does not require treatment. However, it is essential to make sure that this is not a symptom of something serious.
A sudden change of size in your pupils can occur from:
- Head trauma
- Certain medications
- Other medical conditions
Be sure to speak with your doctor immediately if you notice a sudden change in your pupil size. This could be a sign of something serious.
Scheduling regular routine eye exams is essential for your eye health. With regular eye checks, your doctor can monitor your vision continually and inform you of any changes.
Regular visits to your eye doctor can prevent severe problems by recognizing early signs and symptoms.



