Key Takeaways
- Petechiae are small red dots that usually appear around the eyes
- They can be caused by activities, illnesses, and medicines
- Petechiae aren't indicative of eye disease and are not typically dangerous
- See a doctor immediately if you experience fever, vomiting, headache, etc.; it may indicate an underlying condition
- Petechiae are preventable
- Talk to your doctor for home remedies or prescription medication to treat the root cause of the problem
What are the Red Dots Around My Eyes (Petechiae)?
Petechiae are tiny red dots under the eyes, less than 2 mm in diameter. They resemble a rash and can also look purple or brown.
Aside from under the eyes, petechiae can also appear on the neck or the chest. They can also show up as dark brown spots on darker skin tones.
Red dots around the eyes usually aren’t a symptom of anything serious. However, there are times when they can indicate a serious medical concern.
Pictures of Petechiae
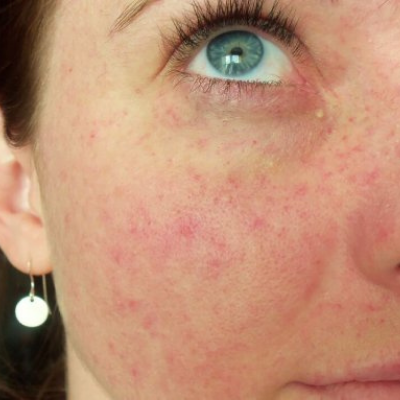
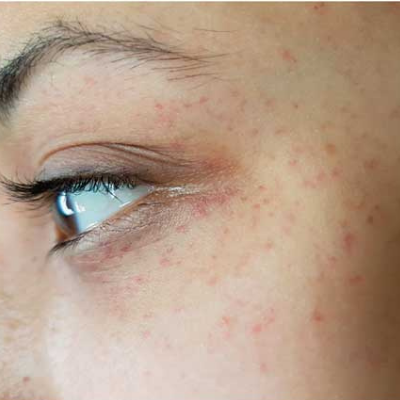
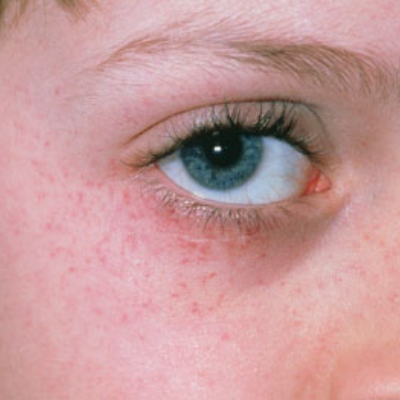
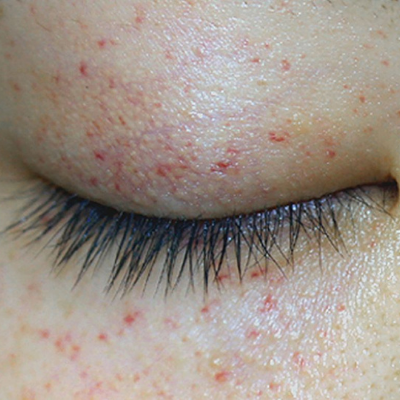
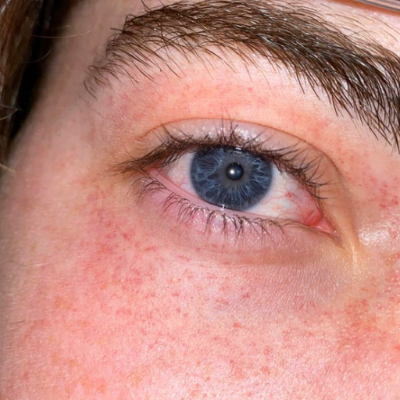
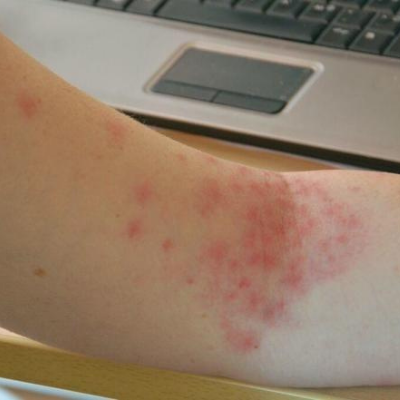
Can Petechiae be a Sign of Something Serious?
A study showed that 25% of people who developed a fever and petechiae on their upper torso had a bacterial infection.5 In most cases, petechiae are one of many symptoms indicating a serious condition.
If a child develops petechiae with a fever, seek immediate medical attention.
When to Seek Help
Contact your doctor immediately if you develop red spots while experiencing:
- A fever of 100.4 or higher
- Vomiting
- Headache
- Stiff neck
- Streaks under your nails
- Trouble breathing
- Sleepiness or fatigue
- Drastic mood changes, especially in children
Seek medical help if you notice the spots are turning into purpura. Blood clots or bleeding into the skin can also be a concern when red dots appear underneath the eyes.
Sick children who develop petechiae or purpura should also seek immediate medical care. Meningococcal infection is a common cause of petechiae in 50% to 70% of cases.4
Listen In Q&A Format
What is Petechiae?
Vision Center Podcast
What Causes Petechiae?
Different things can trigger petechiae. Their appearance is typically attributed to bleeding beneath the skin.
Other potential causes for petechiae include:
- Strong coughing
- Vomiting
- Labor and childbirth
- Lifting heavy weights
- Viral infections (cytomegalovirus (CMV), endocarditis, and mononucleosis)
- Bacterial infections (meningitis, Rocky Mountain spotted fever, scarlet fever, and strep throat)
- Small blood vessel inflammation (Henoch-Schonlein purpura)
- Sepsis
- Viral hemorrhagic fevers (dengue, Ebola, and yellow fever)
- Blood and immune disorders (leukemia, thrombocytopenia, and vasculitis)
- Lack of vitamins C, K, or B12
Can Medication Cause Petechiae?
Yes, you may develop red dots around your eyes because of a reaction to certain medications. These medications include:
- Penicillin
- Quinine
- Seizure medications
- Blood thinners
- Antidepressants
- NSAIDs
- Sedatives
- Heart rhythm drugs
Difference Between Petechiae and Purpura
The main difference between petechiae and purpura is their size. Purpura is larger and is the result of petechiae joining together. Unlike petechiae, purpura spots can merge together, creating larger patches of discolored skin.
Petechiae and purpura are caused by blood vessels breaking under the skin. They can also indicate other health concerns if a person is sick. While similar factors cause petechiae and purpura, the latter is generally linked to more significant bleeding beneath the skin.
Since purpura is larger and potentially indicates more severe bleeding, healthcare professionals take this condition more seriously. You'll require a more thorough medical evaluation and additional diagnostic tests to identify and address the underlying cause.
Petechiae Treatment
Petechiae usually resolve on their own after about two to three days. In some cases, doctors prescribe the following to treat petechiae:
- Corticosteroids
- Antibiotics
- Immunosuppressants
- Vitamin C supplements
These medicines treat infections and reduce inflammation. Doctors may also refer you to a specialist if they suspect your petechiae is related to another disease. For instance, if red dots are caused by skin conditions or an allergic reaction, you might need to see a dermatologist for treatment.
At-Home Petechiae Remedies
Some home remedies prevent spots or help them quickly ease after they form. These include:
- Cold compresses. Applying a cold compress to the affected area helps reduce inflammation and eases the appearance of petechiae
- Rest, relaxation, and plenty of water. If petechiae aren't linked to an infection or underlying condition, resting is important to help the dots subside
- Over-the-counter pain relievers. Medications like acetaminophen and ibuprofen can help with discomfort and pain associated with petechiae
How to Prevent Petechiae Around the Eyes
Identifying the underlying cause of petechiae helps avoid and treat it. However, prevention may not be possible if the dots are related to an illness.
Here are some tips on how to prevent petechiae around the eyes:
- Regularly clean and disinfect countertops, doorknobs, and other surfaces
- Wash your hands frequently with soap and water for at least 20 seconds
- Avoid people who are sick
- Avoid too much sun exposure and wear sunscreen when you go outside
- Discuss possible alternative medication options with your doctor if petechiae is a side effect of your current treatment
- Don't share personal items, such as toothbrushes and razors, with others
- Use an insect repellent when going to grassy or wooded areas
- If you develop petechiae after vomiting or coughing violently, do what you can to avoid these activities
Petechiae can sometimes be confused with other eye conditions. If you notice a single red spot on your eye rather than multiple small dots around the eye, the cause may be different.
Summary
Petechiae are small red dots that appear around the eyes due to bleeding under the skin. They usually resolve on their own within two to three days. Common triggers include strong coughing, vomiting, and certain medications. See a doctor immediately if petechiae appear alongside fever, headache, or stiff neck, as this may indicate a serious infection.



