Primary open-angle glaucoma is a progressive eye disease caused by elevated intraocular eye pressure (IOP).
This condition gradually damages the optic nerve, the connection pathway between the eye and the brain. Glaucoma also damages retinal ganglion cells. These cells transmit visual information from the retina to the brain via the optic nerve.
If left untreated, open-angle glaucoma results in blindness.
Open-angle glaucoma is the most common type of glaucoma. It affects 3 million Americans and is the second leading cause of blindness worldwide.1
Understanding Glaucoma
Glaucoma is an umbrella term for eye conditions caused by increased IOP. The eye is filled with aqueous humor (clear fluid). This fluid is responsible for eye shape and providing the rest of the eye with nutrients and oxygen.
The flow of eye fluid is a continuous process that occurs through a small space called the drainage angle. This space is located between the iris and sclera.
When the drainage angle is blocked or clogged, it leads to increased IOP. This causes damage to the optic nerve, leading to glaucoma.
Listen In Q&A Format
What Is Primary Open Angle Glaucoma
Vision Center Podcast
Open-Angle Glaucoma Symptoms
Open-angle glaucoma progresses slowly over time. It’s usually asymptomatic until its advanced stages when the optic nerve is damaged.
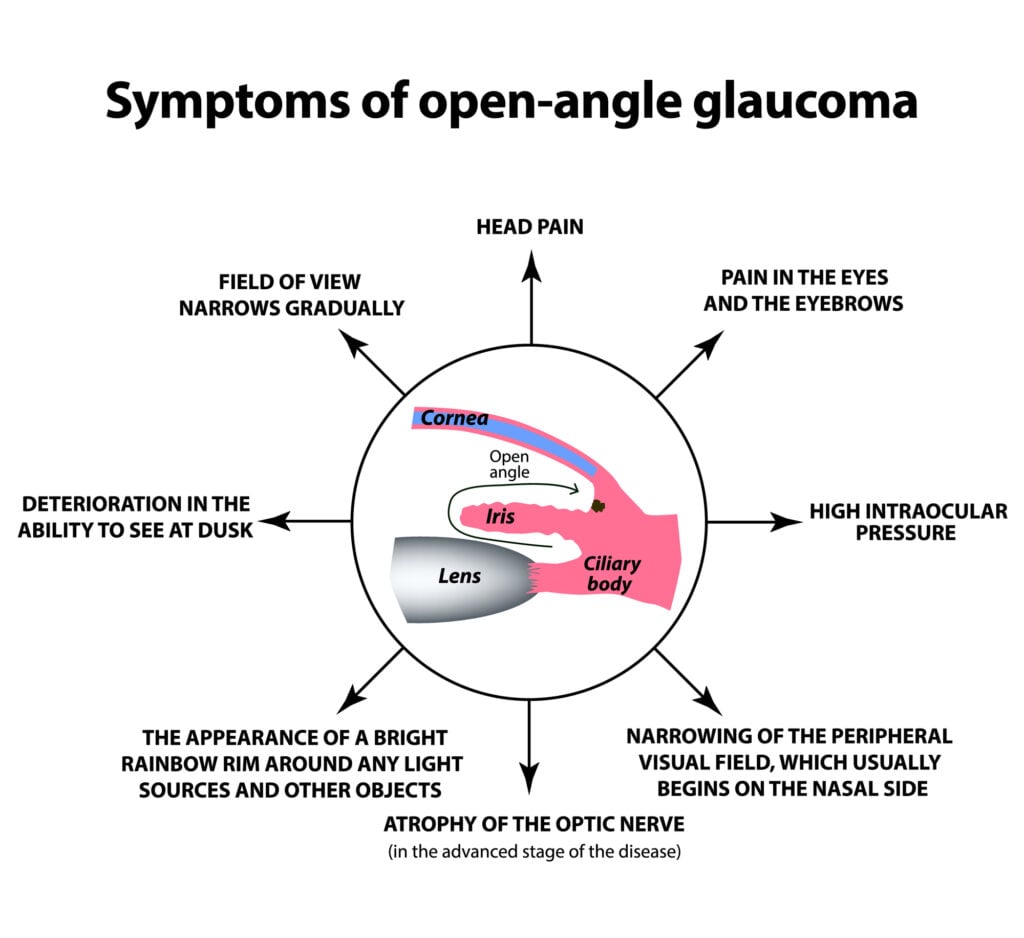
This condition is called the “silent thief of sight” because many people don’t know they have increased eye pressure until their peripheral vision (side vision) changes.
Late-stage symptoms of open-angle glaucoma include:
- Blurred vision
- Blindspots in central vision
- Decreased color vision
- Reduced night vision
- Tunnel vision
Open-Angle vs. Closed-Angle Glaucoma
Glaucoma results from the drainage angle becoming blocked or clogged. This slows down the flow of eye fluid and increases eye pressure.
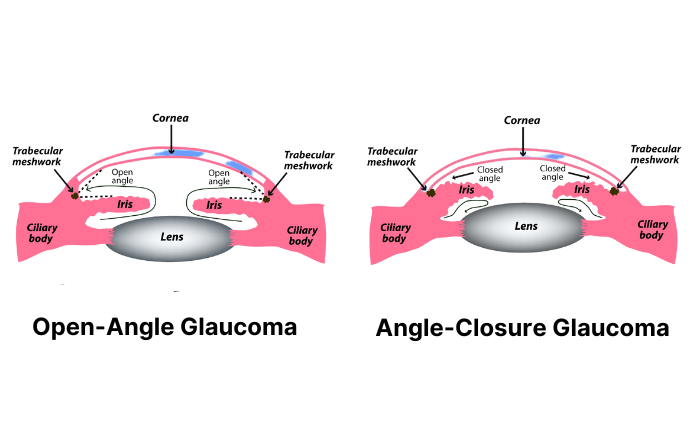
With primary open-angle glaucoma, the trabecular meshwork (spongy tissue in the drainage angle) slowly becomes clogged. This results in a backup of eye fluid, causing eye pressure to increase.
Closed-angle glaucoma is a sudden spike in IOP caused by the iris blocking the drainage angle. Other terms for this condition include acute angle-closure glaucoma and narrow-angle glaucoma.
Symptoms of closed-angle glaucoma include:
- Sudden blurred vision
- Severe eye pain
- Headache
- Nausea and vomiting
- Rainbow halos around light
Closed-angle glaucoma is a medical emergency that requires immediate treatment before it causes irreversible blindness.
Other Types of Glaucoma
A variety of eye conditions that increase IOP can cause glaucoma.
Other types of glaucoma include:
- Normal-tension glaucoma (optic nerve damage without a rise in IOP)
- Secondary glaucoma (caused by medical conditions, eye injury, or medications)
- Pigmentary glaucoma (flakes of pigment block the drainage system)
- Congenital glaucoma (high eye pressure at birth)
- Exfoliative glaucoma (flaky material falls off into the trabecular meshwork, causing elevated IOP)
- Uveitic glaucoma (inflammation of the iris)
- Traumatic glaucoma (caused by eye injury or blunt force trauma)
Causes of Open-Angle Glaucoma
Open-angle glaucoma is caused by increased IOP. This results in optic nerve damage, which eventually causes vision loss.
The drainage angle stays open, but the trabecular meshwork becomes more rigid. This slows down the flow of eye fluid and increases eye pressure.
Risk Factors for Open-Angle Glaucoma
While anyone can develop glaucoma, certain people have increased risk factors, including people who have the following characteristics:
- Are over age 40
- Have a family history of glaucoma
- Experience severe nearsightedness
- Are of African, Hispanic, or Asian descent
- Have a history of eye injury
- Experience thinning of the cornea
The following conditions can also increase risk factors:
- Diabetes
- Migraines
- High blood pressure
- Long-term steroid use
Can You Prevent Open-Angle Glaucoma?
There is no cure for glaucoma, and optic nerve damage is permanent. However, there are steps you can take to detect glaucoma early and manage eye health. Steps include:
- Get a routine comprehensive eye exam from a licensed eye doctor
- Wear eye protection
- Control blood pressure and blood sugar
- Know your family history
- Take prescribed daily eye drops for high eye pressure
When to See an Eye Doctor
Visit an eye doctor right away if you experience vision changes or other symptoms of glaucoma, including:
- Sudden vision loss
- Severe eye pain
- Headache
- Difficulty focusing
- Blindspots in your peripheral (side) or central
Routine eye exams are essential if you are at high risk of developing glaucoma.
How is Open-Angle Glaucoma Diagnosed?
A licensed ophthalmologist can diagnose open-angle glaucoma during a comprehensive eye exam. During the exam, the eye doctor will measure IOP using a tonometry test or an “eye puff” test.
They will use specific eye drops to dilate your eyes. This helps them to examine the following for signs of disease:
- Retina (layer in the back of the eye that sends light messages to the brain)
- Optic nerve and optic nerve head
- Other eye structures
Other eye tests that can help diagnose or monitor glaucoma include:
- Visual field test of the side and central vision
- Optical coherence tomography images your optic nerve to check for damage
- Visual acuity test to examine clarity and distance vision
- Measure corneal thickness
Can an Open-Angle Glaucoma Diagnosis Be Incorrect?
In some cases, the diagnosis of open-angle glaucoma can be incorrect. It can be challenging due to its resemblance to other eye conditions, potentially leading to incorrect diagnoses.
Your doctor may also miss the symptoms of glaucoma, especially if they aren’t looking for the disease. To ensure accurate detection and timely intervention, it’s crucial to undergo regular eye examinations.
Open-Angle Glaucoma Treatment Options
Glaucoma can’t be cured or reversed. However, there are effective treatment options that help slow its progression and preserve vision.
The first goal of treating open-angle glaucoma is reducing IOP to minimize optic nerve damage. Treatment options include medication, laser therapy, and surgery.
Medication
Medicated eye drops can control eye pressure. You will most likely need to administer daily eye drops for the rest of your life. In some cases, laser or surgery can reduce the need for drops.
Prescribed eye drops for glaucoma include:
- Beta-blockers to reduce eye fluid production
- Prostaglandins to increase outflow
- Alpha-adrenergic agonists to reduce eye fluid production and increase outflow
- Miotic or cholinergic agents to increase eye fluid outflow
Laser Therapy
If medication does not lower eye pressure, laser surgery can repair the drainage angle. This will restore the continuous flow of eye fluid.
Trabeculoplasty is laser surgery that treats open-angle glaucoma. It unclogs the drainage angle. This allows eye fluid to flow continuously and decreases eye pressure.
Glaucoma Surgery
Traditional glaucoma surgery is used when medication is ineffective in reducing IOP. Glaucoma surgery aims to repair the drainage system and unclog the trabecular meshwork.
Types of glaucoma surgery used to treat open-angle glaucoma include:
- Trabeculectomy, which creates a tiny flap in the sclera and drainage reservoir for eye fluid
- Glaucoma drainage device, which is a small implanted tube used to drain eye fluid
- Cataract surgery, which implants an artificial lens to correct narrow angles
Outlook
While glaucoma is irreversible, it can be treated to slow disease progression and minimize vision loss.
Catching open-angle glaucoma in its early stages is the best way to preserve vision and reduce complications, including blindness.
A routine comprehensive eye exam is the best way to diagnose glaucoma early.
Summary
Open-angle glaucoma is the most common type of glaucoma. A clog in the drainage angle causes it, which disrupts the flow of eye fluid and increases eye pressure and optic nerve damage.
Open-angle glaucoma is a slow-progressing disease that doesn’t produce symptoms until advanced stages. This makes catching it early difficult. Warning signs of glaucoma include blurry vision and blind spots in peripheral (side) vision.
While it can’t be cured, open-angle glaucoma can be treated and managed with medication, laser therapy, and glaucoma surgery.



