It’s common to experience dry eye occasionally during sunny, less humid, windy weather or if you have vision-related allergies. However, this can escalate from a one-time occurrence to a chronic illness that demands medical attention.
Any condition that disrupts the formation of tears in the tear film and drainage into the tear ducts causes dry eye syndrome. This article will discuss the following:
- What is dry eye syndrome?
- How the condition is diagnosed
- Available treatment options
- Alternative remedies
Listen In Q&A Format
Dry Eye Treatment: Effective Remedies \u0026amp; Solutions
Vision Center Podcast
What is Dry Eye Syndrome?
Dry eye syndrome (DES) or dry eye disease (DED) presents as insufficient tears in the eyes.1 The tear film has three layers that protect the eye and help you see clearly and comfortably.
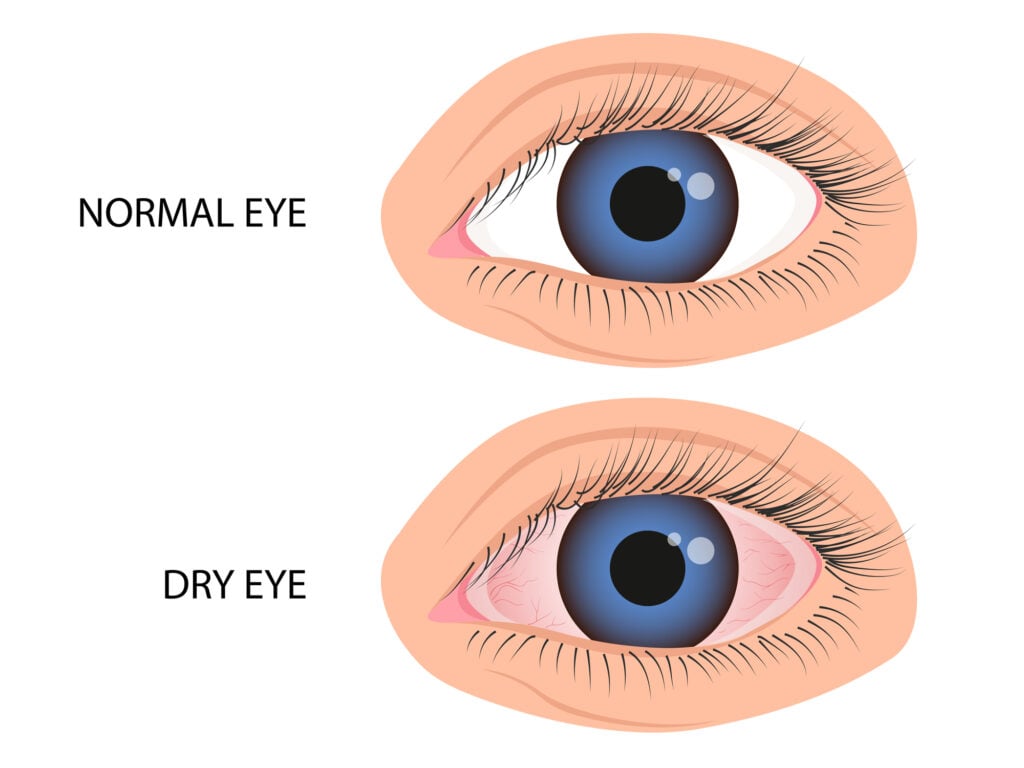
DES affects the integrity of the tear film, leaving your eyes unprotected. It can result from underlying health conditions or eye injury.
Other names of dry eye syndrome are:
- Keratoconjunctivitis sicca (KCS)
- Dysfunctional tear syndrome
- Lacrimal keratoconjunctivitis
- Evaporative tear deficiency
- Aqueous tear deficiency
- LASIK-induced neurotrophic epitheliopathy (LNE). (A side effect of LASIK surgery)
Prevalence
DES is more prevalent among people over 40, with high risk among those aged 45-54. More women than men suffer from dry eyes due to oral contraceptives, pregnancy, and menopause.2
According to a National Health and Wellness Survey, 6.8 percent of the U.S. adult population (about 16 million) have been diagnosed with dry eye syndrome.
Symptoms of Dry Eye Syndrome
The common symptoms of dry eye include the following:5
- Feeling like there’s an object in your eye
- Blurred vision
- Inflammation
- Red eyes
- Burning sensation
- Itchiness
- Stringy mucus at the corner of the eye
- Excessively watery eyes
- Sensitivity to light (photophobia)
- Eye fatigue (tired eyes)
- Pain and difficulty opening your eyelids when waking up
Most people with minor symptoms tend to ignore them until they experience visual difficulties when performing daily tasks. If you suspect dry eyes, visit your eye doctor for further examination. Early treatment will prevent the condition from progressing.
Types of Dry Eye
There are three types of dry eye syndrome:
Evaporative Dry Eye (EDE)
Tears have an oil (lipid), mucus, and water layer. The water layer holds the tears, the oil layer prevents evaporation of the tears, and the mucus layer maintains an even tear film.
Conditions like meibomian gland dysfunction (which occurs in over 85% of cases of dry eyes) affect the function of the oil layer, causing quick evaporation of the water layer.
Aqueous Deficient Dry Eye (ADDE)
Aqueous deficient dry eye means insufficient tear production. The lacrimal gland present at the top outer corner of each eye produces and stores the aqueous solution.
Some conditions can damage the tear gland and interfere with tear formation. These include:
- Sjögren’s
- Sarcoidosis
- Lupus
- Rheumatoid arthritis
Mixed Dry Eye (MDE)
This type of dry eye combines both types discussed above. In this case, a person has insufficient tear production, and the little tears they produce evaporate quickly.
Causes and Risk Factors of Dry Eye Syndrome
Dry eyes result from insufficient tear formation or decreased quality of the tears. The following factors predispose you to develop dry eyes:
- Eye injuries. Corneal abrasions are also linked to dry eyes.3
- Poor blinking habits. This is common when reading or looking at a computer screen for extended periods.
- Contact lenses. Contact lens wearers are at risk of dry eyes due to limited oxygen and tear flow in the cornea.
- Aging. Most people over age 65 are likely to experience dry eye symptoms.
- Medications. Certain drugs such as antihistamines, heart medications, birth control pills, diuretics, and ulcer medications can affect tear formation.
- Underlying medical conditions: People with diabetes, rosacea, Sjögren’s syndrome, lupus, scleroderma, and rheumatoid arthritis are likelier to suffer from dry eye.
- Environmental factors: Prolonged exposure to sunlight, wind, smoke, and dry climate increase the evaporation of the tears, resulting in dry eyes.
- Surgeries: Undergoing some surgeries like LASIK, corneal, and cataract surgery solves the underlying condition but results in dry eyes by interfering with tear formation.
- Lifestyle: Spending long hours on screens like mobile phones, computers, laptops, or tablets increases your chances of getting dry eye syndrome. Allergies, smoking, and contact lenses also significantly influence dry eye risk.
- Cosmetic products: Studies show that ingredients used in cosmetics and beauty care products like mascara, eye-shadow, and eyeliner are harmful and can cause dry eyes if they migrate to the eye's surface.4
- Eyelid conditions: Eyelid disorders like lower eyelids turning outwards (ectropion) or inwards (entropion) can cause friction, cornea irritation, and exposure leading to dry eyes.
How is Dry Eye Syndrome Diagnosed?
If your doctor suspects dry eyes, they will perform several tests to confirm the condition. They’ll begin by examining your medical history and determine if your symptoms align with dry eye syndrome.
They will examine the following:
- Symptoms you have experienced and the duration
- Exacerbating and relieving factors
- Other symptoms like dry mouth, fatigue, joint pain, and oral ulcers.
- History of eye surgeries
- History of related eye diseases
- Use of contact lenses
- History of underlying chronic illness
- Smoking habits and exposure to passive smoke
After assessing your medical history, your eye doctor will conduct a comprehensive eye examination to evaluate the lid structure, cornea, and blink dynamics. Under magnification, the eye doctor assesses the tear layers; outer lipid, middle aqueous, and inner mucin layer.
Tear Assessment Tests
Your eye care provider will conduct several tests to diagnose dry eye syndrome, as there isn’t a single conclusive test. Some tests are:
1. Tear Breakup Time (TBUT) Test
TBUT test evaluates the tear evaporation rate. The eye doctor puts dye in your eyes and observes how long the tear film will remain stable under the microscope.
They may also use a special device known as LipiView Ocular Surface Interferometer to take photos and assess the tear film.
2. Slit lamp exam
The slit lamp magnifies and focuses high-intensity light on the eye's structures to determine any damage. These include:
- Iris
- Cornea
- Vitreous humor
- Eyelids
- Conjunctiva
- Sclera
3. Schirmer’s test
During this test, the eye doctor places paper strips along the edge of your lower eyelid. This test estimates the volume of tears your lacrimal glands produce.
4. TearLab Osmolarity System (TearLab) test
This test measures tear osmolarity, which, if too high, may damage the cornea and conjunctiva. This test is quicker and less invasive than Schirmer testing.6
5. Meibomian gland evaluation
This test measures the integrity of the Meibomian glands and whether enough oil is secreted to lubricate the eye and reduce tear evaporation.
6. Epithelial staining
Your healthcare provider uses an eye dropper to add a yellow dye to your eyes. The dyes help determine how quickly the tears dry and highlight any epithelial damage on the eye’s surface.
What Are the Treatment Options for Dry Eye Syndrome?
Managing dry eye syndrome can be categorized into supportive and definitive treatment.7
- Supportive management. Aims to ease the symptoms of dry eye syndrome and minimize further damage.
- Definitive treatment. Treatments are based on the severity and management of the underlying illness
Supportive Management
The following are supportive management measures for DES:
- Artificial tears. To create an artificial tear film that lubricates the eye and improves comfort. Use preservative-free artificial tears as the chemical preservative added to the drop to prevent bacterial growth can damage the eye’s epithelial tissue over time.
- Tear conservation. Refers to maintaining the secreted tears longer without evaporating. One way is sealing the puncta (where the tears drain) in a process known as punctal occlusion. There is also a surgical procedure known as cautery. It uses heat to close the ducts permanently.
- Blinking more often helps keep the tear film intact for longer durations. When your eyes are glued to a book or screen, you blink less, and the tears evaporate faster, leaving the eyes dry.8
- Eye gels and ointments. These are denser than artificial tears, creating lasting effects. Apply the gel or ointment before bed and shut your eyes for at least 15 minutes. Avoid using the ointments during the day, as they can blur your vision.
- Eyelid scrubs. Used to scrub away the debris on your eyelid. A clean eyelid keeps the tear glands healthy, improving tear secretion and drainage. Tea tree oil solution is a safe, popular eyelid cleaner you can make yourself.
- Humidifier. If you live in low-humid areas, a humidifier increases the moisture level in your space, reducing the tear evaporation rate.
- Dry eye glasses. These comfortably wrap and protect the eye sockets from dust, winds, and sunlight. They also relieve symptoms of dry eyes.
- Quitting smoking. Cigarette smoke contains chemicals that can affect your eyes. The less you smoke, the less inflamed and dry your eyes become.
- Remove and replace your contact lenses. Use disposable daily contact lenses to prevent the build-up of dirt and bacteria. Also, avoid sleeping in your contact lenses at night to let your eyes breathe.
- Warm compresses. The heat from a warm compress pad/towel will open the meibomian glands, thus improving oil gland function. It also increases oil flow into the eyes and stabilizes the tear film.9
- Give your eyes a break. Do this by taking breaks from bright screens and reducing eye strain. Also, take a break from using mascara, eye shadow, and eyeliner to avoid damaging your Meibomian glands.
Definitive Treatment
Definitive treatments for dry eyes include the following:
- Anti-inflammatory drugs. These are topical medications prescribed to ease the discomfort of dry eye syndrome. Common examples are cyclosporine (Restasis®) and Lifitegrast (Xiidra®)
- Medical adjustments. Your doctor may recommend this if the drugs you are using are causing dry eyes. These may include antidepressants, hypertension medication, oral birth control pills, and antihistamines**.**
- Managing underlying conditions. Treating conditions that cause dry eyes, like diabetes, thyroid disorders, or rheumatoid arthritis, eases dry eye syndrome.
- Medical procedures. Thermal Pulsation therapy (Lipiflow) involves massaging the dysfunctional meibomian glands to stimulate the glands to produce oil. Intense pulsed light (IPL) therapy liquefies the oils that have solidified and clogged the meibomian gland.
- Punctal occlusion. This is a painless procedure involving punctal blockage to suppress quick tear drainage. You can opt for temporary plugs or permanent silicone plugs that last as long as you need.
- Autologous blood serum drops (AS). An effective dry eye treatment using blood serum. In this case, your serum is used to customize your artificial tears. Unfortunately, this procedure is expensive, and your insurance provider may not cover it.10
- Nasolacrimal treatments. FDA- approved treatments like Tyrvaya (nasal spray) and iTear100 (neurostimulator device) stimulate the production of natural tears.
- Therapeutic contact lenses. Soft bandage lenses prevent damage to the cornea (corneal abrasions), and rigid scleral lenses protect the cornea and sclera (whites of the eye).
- Amniotic membranes and drops. These are placed over the eyes to reduce inflammation. Amniotic membranes are rich in anti-inflammatories and growth hormones, stimulating ocular surface repair.11
Comparing Treatment Options
| TREATMENT | PURPOSE | SIDE EFFECTS |
|---|---|---|
| Cyclosporine A 0.05% emulsion (Restasis) | FDA-approved for increasing tear production | Visual blurring / Burning sensation |
| Lifitegrast Eye Drops (Xiidra) | Treats ocular surface inflammation | Allergic reactions |
| Varenicline nasal spray (Tyrvaya) | Stimulates tear production and reduces the tear evaporation rate | Sore throat / Nose irritation |
| Autologous serum | Treats ocular surface inflammation that cause dry eye | Risk of microbial growth |
| Non-steroidal anti-inflammatory drugs (NSAIDs) | Manage postoperative ocular pain and any other dry eye-related pain | Impairs wound healing / Can cause corneal epithelium damage |
Treating the Underlying Causes of Dry Eye Syndrome
Proper management of underlying conditions like diabetes, arthritis, menopause, or thyroid disorders helps reduce symptoms of dry eyes. Treating a problem from the source is more important than treating its symptoms.
For example, if the cause of your dry eyes is ectropion or entropion (outward turning of the eyelid), your oculoplastic surgeon might suggest surgical interventions to correct the eyelid and prevent overexposure of the eyeball to external conditions.
Alternative Remedies for Dry Eye Syndrome
If you prefer natural remedies instead of taking a pill or eye drops, here are some options you can try:
- Omega-3 fatty acids. Found in foods like fish, sardines, and flaxseeds. Add fatty acids to your diet to promote good eyesight and reduce dry eye symptoms.
- Water intake. It keeps the body hydrated, which is excellent for tear production.
- Vitamin D supplements. Vitamin D nutrient supports tear production and strong eyesight. The supplements are suitable for people who don’t get sufficient vitamin D from the sun.
- Vitamin A-rich food sources. Foods like carrots, oranges, vegetables, and fortified skim milk boost good eyesight and enrich the ocular surface preventing dry eyes.
- Lutein and zeaxanthin. Found in vegetables like kale, spinach, silverbeet, and romaine lettuce, these antioxidants keep the body’s cells healthy and functioning correctly. This way, they prevent chronic eye illnesses like dry eyes.12
- Zinc minerals. Zinc comes from sources like nuts, legumes, meats, and dairy. Zinc is responsible for transporting vitamin A from the liver to the retina.
- Acupuncture. Recent studies have shown an improvement in dry eye symptoms using true acupuncture. The procedure can relieve the symptoms of dry eyes and generally improve eye health.13
- Castor oil eye drops. These nourish the eyes with oil and water, reducing tear evaporation.
Common Questions about Dry Eyes
Here are answers to some frequently asked questions about dry eye syndrome:
Can dry eyes be cured?
No. Scientists haven’t found a cure for dry eyes yet. The best solution for dry eye syndrome is the management of symptoms to reduce the severity and progression.
What’s the leading cause of dry eyes?
There are several causes of dry eyes, including prolonged contact lens use, poor blinking habits, certain medications, and underlying conditions such as diabetes, rheumatoid arthritis, lupus, and Graves' disease.
What’s the most effective medication for dry eyes?
Ophthalmologists recommend long-term use of prescription eye drops like cyclosporine (Restasis®) and lifitegrast ophthalmic solution (Xiidra®) to reduce inflammation, itchiness, and redness from dry eyes. The drops also work as lubricants and maintain the tear film.
Does drinking water help my dry eyes?
Drinking enough water keeps the body hydrated and supports natural tear production. Diuretics and drinks like caffeine can contribute to dehydration and interfere with tear formation.
Summary
- Dry eye syndrome (DES) or dry eye disease (DED) presents as insufficient tears in the eyes.
- DES is more prevalent among people over 40, with high risk among those aged 45-54.
- Common symptoms of dry eyes include eye discomfort, blurry vision, photophobia, excess tears, etc.
- Your eye doctor can perform a series of tests to determine the cause and extent of your dry eye disease.
- Common treatments include lubricating eye drops, anti-inflammatory medications, and treatments for underlying conditions.
- Alternative remedies like acupuncture, supplement intake, proper diet, and proper hydration can also help manage dry eyes.



