Key Takeaways
- A cherry red spot is a small, reddish area on the eye's macula. It appears red due to the surrounding opacified retina.
- There are many possible causes of macular cherry red spots, including central retinal artery occlusion (CRAO) and lipid storage diseases.
- Most causes are severe medical conditions, and some involve a short life expectancy.
- Cherry red spots may occur with sudden-onset, painless loss of vision. If this happens, seek immediate medical treatment.
What is a Cherry Red Spot?
A cherry red spot is a small reddish area in the center of the eye's macula. The retina surrounding the red spot is generally opaque.
This red-tinted spot is visible through the transparent tissue of the macula, which is the area of greatest visual acuity. It appears as a cherry red spot because the whitish, opaque retina surrounding it obscures the blood vessels at the back of the eye.
If your eye doctor sees a cherry red spot during an eye examination, they will investigate it to determine the underlying cause.
Conditions that can cause cherry red spots are:
- Mucolipidosis type I (sialidosis)
- Central Retinal Artery Occlusion
- Niemann-Pick Disease
- Tay-Sachs Disease
- GM1 Gangliosidosis
- Sandhoff disease
What Does a Cherry Red Spot on Macula Look Like?
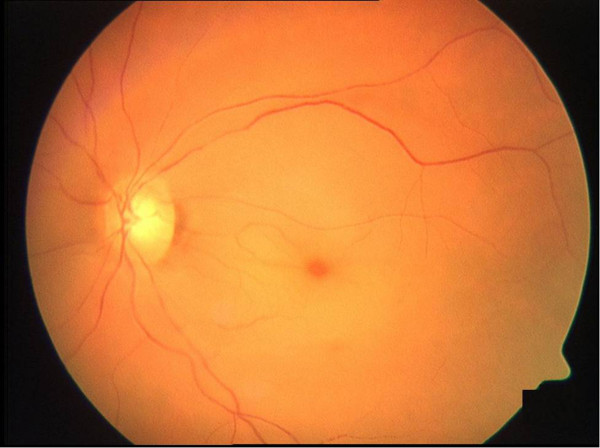
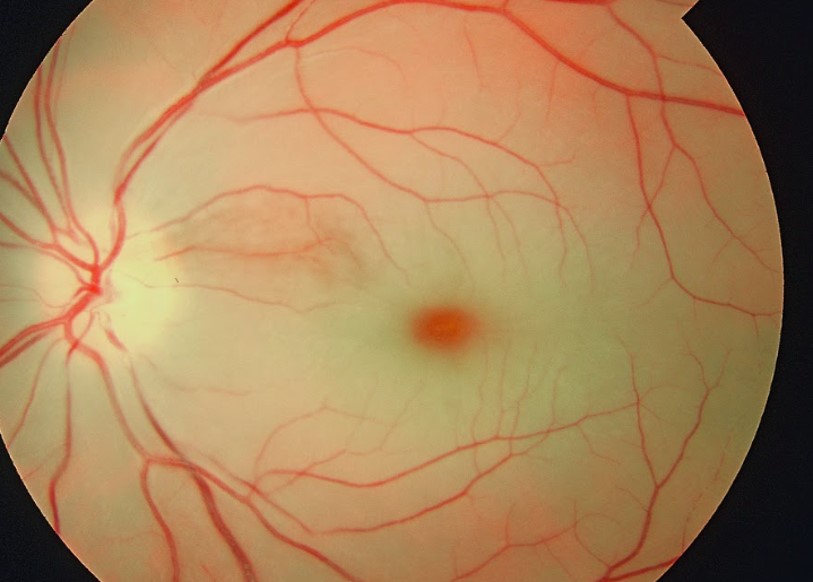
What Causes a Cherry Red Spot on the Eye?
The causes of a macular cherry red spot fall into five categories:
- Vascular
- Metabolic storage diseases
- Toxicity
- Ocular trauma
- Inflammation
Vascular
Central retinal artery occlusion (CRAO) is an eye disease that involves blocked blood flow through the central retinal artery. CRAO has many possible causes, but carotid artery atherosclerosis is the most common.
90% of people with permanent CRAO had a cherry red spot during their initial examination.2
Metabolic Storage Diseases
Metabolic storage diseases are a group of rare genetic disorders that cause enzyme insufficiencies. Enzymes help break down materials needed for proper cellular functioning.
Cherry red spots can occur with the following metabolic storage diseases:
Tay-Sachs Disease
Tay-Sachs disease is a genetic disorder that destroys brain and spinal cord (central nervous system) cells. Babies born with this disease show symptoms during infancy.
A cherry red spot is present in about 90% of children with Tay-Sachs disease.2 Other symptoms include:
- Deafness
- Blindness
- Seizures
- Dementia
- Apathy
- Poor head control
- Increased startle response
Most children with this disease have a life expectancy of 2 to 5 years.
Farber Disease
Farber disease is a rare lysosomal storage disorder. A deficiency of the acid ceramidase enzyme causes it. Low enzyme levels cause a fatty material called ceramide to build up in cells.
Ocular symptoms of Farber disease include corneal clouding and cherry red spots. Common symptoms include painful, swollen joints and a weak or hoarse voice.
GM1 Gangliosidosis
Doctors may refer to GM1 gangliosidosis as generalized gangliosidosis or Landing disease. This disease occurs due to a deficiency of beta-galactosidase.
A cherry red spot occurs in about 50% of cases.2
GM2 Gangliosidosis
Doctors may refer to GM2 gangliosidosis as Sandhoff disease. This genetic disorder occurs when the HEXA enzyme mutates at a specific chromosome.
Symptoms are similar to those of Tay-Sachs disease, including the macular cherry red spot.
Niemann-Pick Disease
Niemann-Pick disease is a group of severe metabolic disorders. They cause an accumulation of sphingomyelin (a type of sphingolipid) in the tissues.
This disease has four different types:
- Type A: This disease affects babies and involves severe neurodegeneration. Most people with this type have a cherry red spot at the macula.
- Type B: Occurs mid-childhood and is less severe than type A. About 33% of cases involve cherry red spots.
- Type C and D: These types appear slowly. They cause progressive but severe damage to the central nervous system.
Metachromatic Leukodystrophy
This lysosomal storage disease causes the progressive destruction of white matter in the brain. People with this condition occasionally have a cherry red spot.
Metachromatic leukodystrophy leads to a progressive decline in intellectual and motor functions, including:
- Hearing loss
- Blindness
- Loss of speech
- Loss of mobility
- Unresponsiveness
- Death
Sialidosis
This lysosomal storage disease is called mucolipidosis type 1 or cherry red spot myoclonus syndrome. People with sialidosis have a deficiency of neuraminidase 1 (NEU1) or sialidase (SIAL1) enzymes.
Almost all people with sialidosis have a macular cherry red spot. Other symptoms include:
- Gait disturbance (issues walking)
- Myoclonus (involuntary muscle twitching or jerking)
- Tremors
- Seizures
- Ataxia (difficulties in balance and coordination)
Toxicity
Cherry red spots may result from toxic levels of certain substances. These include:
- Quinine
- Carbon monoxide
- Methanol
- Dapsone (antibiotic)
Ocular Trauma
Physical or chemical injuries that damage the eye can cause cherry red spots. This includes:
- Blunt trauma (getting hit in the eye)
- Anesthetic injections behind the eyeball
- Complications from cataract surgery
Retinal Inflammation
Inflammation of the retina, called retinitis, can cause cherry red spots if it affects the central retina. Retinal disorders that cause this type of inflammation include:
- Progressive outer retinal necrosis
- Subacute sclerosing panencephalitis
Risk Factors
People with central retinal artery occlusion (CRAO) will likely develop macular cherry red spots.
These conditions increase your risk for CRAO:
- Carotid artery atherosclerosis (leading cause)
- Cardiogenic embolism
- Hematological conditions, such as sickle cell disease, leukemia, and lymphoma
- Vascular diseases like carotid artery dissection, Fabry disease, and Moyamoya disease
- Giant cell arteritis
Other factors that increase your risk for cherry red spots include:
- Drug use
- Smoking
- Ocular trauma
- Face-down surgical procedures
- History of temporary vision loss
- Medical history of cardiovascular disease or cerebrovascular disease
- Family history of lipid storage disorders or metabolic disease
Symptoms of Cherry Red Spots
People with macular cherry red spots may experience sudden, painless vision loss that lasts several seconds.
Other symptoms vary depending on the underlying cause but may include:
- Transient migraine headaches
- Neurological symptoms of lysosomal storage disorders
- Symptoms of giant cell arteritis, such as headache, scalp tenderness, and muscle and joint pain
If you experience sudden vision loss, call your eye doctor right away.
Diagnosis
Because many diseases can cause a cherry red spot, proper diagnosis may involve a team of medical professionals. People diagnosed with central retinal artery occlusion (CRAO) may need an urgent neurology exam to check for stroke.
An ophthalmologist will perform a fundoscopic exam (fundoscopy). This allows them to examine the back wall of your eye. They’ll check for an opacified retina and red-tinted spot.
A macular cherry red spot is a significant fundoscopic finding, often indicating an ocular emergency. This is especially true if the red spot occurs with sudden, painless vision loss.
Your eye doctor may run additional tests to ensure the red spot isn’t due to another condition, such as:
- Macular hemorrhage
- Macular hole
- Laser injury to the fovea
Tests to confirm the diagnosis may include:
Optical Coherence Tomography (OCT)
This noninvasive imaging test uses reflected light to generate pictures of the back of the eye. It’s commonly used to diagnose diseases like diabetic retinopathy and glaucoma.
Fundus Autofluorescence (FAF)
Like OCT, FAF is also a noninvasive imaging technique. It detects early signs of retinal diseases like age-related macular degeneration.
Fundus Fluorescein Angiography (FFA)
This is an invasive diagnostic procedure that evaluates retinal circulation. It involves injecting a fluorescent dye and using a special camera.
Treatment for Macular Cherry Red Spots
Treatment of a cherry red spot depends on its cause. Healthcare providers will perform a differential diagnosis to provide the appropriate treatment.
CRAO Treatment
If someone has CRAO, treatment options may include:
- Ocular massage
- Anterior chamber paracentesis
- Reduce intraocular pressure with systemic or topical medications
- Hyperbaric oxygen therapy
- Intra-arterial thrombolysis
Metabolic Disorders Treatment
For those with lipid storage disorders, care management may involve treatments like:
- Enzyme replacement therapy
- Symptom control
- Reduction in specific molecule intake
Retinitis Treatment
Treatment for retinitis is individualized based on a person’s unique needs. Options may include topical or systemic steroids.
Prognosis
The outlook for a cherry red spot on the macula depends on the cause. Vision lost due to retinal damage will not improve, even with treatment.
People with CRAO usually experience atrophy of the retina and optic disc. Eventually, they may experience painful blindness.
Other causes of cherry red spots may lead to retinal thinning and retinal detachment.



