Horner syndrome is a rare disorder that affects the eye and face on one side of the body. It usually results from damage to the sympathetic nerve supply from the brain to the eyes.
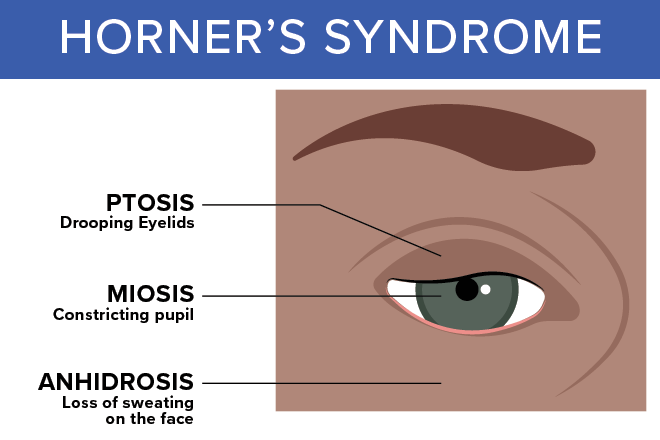
This disruption of nerve function can cause changes in pupil size, a drooping eyelid, and a lack of sweating.
Horner syndrome typically occurs when an underlying medical condition disrupts the sympathetic nerve pathway in the head and neck. In rare cases, it’s present at birth (congenital).
Other names for this disorder include Bernard-Horner Syndrome and oculosympathetic paresis. Horner syndrome is uncommon, affecting about 1 in 6,000 people.6
What are the Symptoms of Horner's Syndrome?
Horner syndrome symptoms usually affect one side of the face. Classic signs and symptoms include:
- Miosis. A constricted pupil that results in mismatched pupil sizes
- Anisocoria. Different pupil sizes
- Partial ptosis. Drooping of the upper eyelid in the affected eye
- Facial anhidrosis. Absence of sweating on the affected side of the face
Rarely, facial flushing may occur on the affected side.
Signs and Symptoms in Children
In children with the congenital form of Horner syndrome, the affected iris will remain the same blue-gray color it was at birth. This leads to different colored irises (heterochromia) as iris pigmentation develops in the first two years.
What Causes Horner's Syndrome?
Horner syndrome is typically caused by damage to the sympathetic nerves that serve your eyes. These nerves carry signals from your brain that cause pupillary dilation and facial sweating.
Sympathetic nerves connect the brain to different parts of the body. The sympathetic nervous system (SNS) triggers involuntary actions in response to dangerous or stressful situations.
Acquired Horner Syndrome
Horner syndrome usually develops when an underlying health condition interrupts nerve function along the sympathetic pathway.
Causes of acquired Horner syndrome vary widely and may include:
- Carotid artery aneurysm or dissection
- Migraine or cluster headaches
- Spinal cord injury
- Tumors
- Stroke
Congenital Horner Syndrome
Congenital Horner syndrome is present at birth. It usually results from birth trauma or a nerve or carotid artery injury.
In extremely rare cases, the condition appears to be inherited. This occurs in only 5% of cases.6
Idiopathic Horner Syndrome
Some people develop Horner syndrome without having a clear underlying cause. This is known as idiopathic.
The 3 Types of Horner's Syndrome
Horner syndrome can involve disruption along three different nerve pathways. For this reason, there are three different types of the disorder with various possible causes.
1. First-Order Horner’s Syndrome
Also known as Central Horner syndrome, it affects the first-order neurons (FON) found along the hypothalamus in the brain and the spinal cord.
Possible causes of damage to this nerve pathway include:
- Neck trauma
- Spinal cord injury
- Multiple sclerosis (MS)
- Meningitis
- Encephalitis
- Interrupted blood flow to the brain stem
- Tumor on the hypothalamus
- Cyst in the spinal column (syringomyelia)
- Lateral medullary syndrome
2. Second-Order Horner’s Syndrome
Also known as preganglionic Horner syndrome, it affects second-order neurons. This pathway runs along the chest, the top of the lungs, and the carotid artery in the neck.
Causes may include:
- A tumor in the upper lungs
- Trauma to the neck or chest from surgery or an accident
- Damage to the aorta
3. Third-Order Horner’s Syndrome
Also known as postganglionic Horner syndrome, it affects the third-order neurons. This nerve pathway runs across the neck, the middle ear, and the eye.
Potential causes include:
- Migraines or cluster headaches
- Middle ear infections
- Damage to the major blood vessels in the neck (carotid artery or jugular vein)
- Infection or tumor near the base of the skull
Is Horner's Syndrome Life-Threatening?
Horner syndrome doesn’t cause significant issues with a person’s vision or overall health.
However, it may be a sign of oculosympathetic nerve damage. Damage to this nerve may result from serious and sometimes life-threatening medical conditions, including cancer and stroke.
When to See a Doctor
See your healthcare provider as soon as possible if you develop symptoms of Horner syndrome. Because it may occur due to serious medical conditions, a prompt and accurate diagnosis is essential.
Seek emergency medical care if symptoms appear suddenly after a traumatic injury on the head or neck or if the following signs accompany them:
- Impaired eyesight
- Dizziness
- Muscle weakness
- Sudden severe headache
- Severe neck pain
How is Horner's Syndrome Diagnosed?
First, your doctor will review your symptoms and take a detailed history. They’ll ask about a history of trauma from surgeries or injuries and any illnesses you’ve had.
They’ll also perform a physical exam, checking your eyelid, pupillary function, and facial sensation.
In addition, they may perform a series of tests to confirm a positive diagnosis and identify the site of nerve damage.
Tests to Confirm Horner Syndrome
An ophthalmologist may confirm the diagnosis by putting special eye drops in both eyes. The drops will cause a normal pupil to dilate or constrict.
By comparing how the two pupils react, your doctor can determine whether nerve damage is the root of the problem.
Tests may include:
Topical Apraclonidine Test
A solution is applied to both eyes to confirm a Horner’s syndrome diagnosis. The affected side will respond with dilated pupils and elevation of the eyelid. Meanwhile, the healthy eye will not respond or experience mild miosis.
Topical Cocaine Test
A cocaine solution is applied to both eyes and checked after 30 minutes. If the affected eye doesn’t dilate as much as the healthy eye, it confirms Horner’s syndrome.
Tests to Identify the Site of Nerve Damage
Tests to determine the location and cause of nerve dysfunction include:
Imaging Tests
These usually check for tumors, lesions, and structural abnormalities. Imaging the cervical spine may help rule out a carotid artery dissection, which can be life-threatening.
Imaging tests include:
- Chest X-ray
- Ultrasound
- Magnetic resonance imaging (MRI)
- Computed tomography (CT)
Blood Tests
Initial lab testing usually includes a complete blood count (CBC) and erythrocyte sedimentation rate (ESR). Additional blood and urine testing may be necessary to determine the underlying cause.
Treatment Options for Horner's Syndrome
Horner syndrome doesn’t have a specific treatment. Instead, medical treatment focuses on addressing the underlying cause.
When appropriate, a doctor may recommend surgical interventions to alleviate conditions such as aneurysms, carotid artery dissection, and tumors.
What is the Recovery Rate/Outlook?
Horner syndrome usually goes away when the underlying medical condition is resolved.
The prognosis depends on the causative factors. While the condition itself won’t affect your eyesight or quality of life, there may be a severe and life-threatening condition causing it that requires immediate treatment.
Summary
Horner syndrome is a rare condition that affects the nerve supply to the eye. Classic clinical signs include partial ptosis (drooping upper eyelid) and an abnormal pupil in the affected eye.
Call your healthcare provider at the first signs of Horner syndrome. It may be due to an underlying condition that needs prompt medical treatment. Horner syndrome usually goes away when the underlying cause is effectively treated.



