What is Milia?
Milia are white, keratin-filled cysts on the skin. They’re also known as skin lesions over 1 to 3 mm in diameter.

People often mistake them for whiteheads or pimples, and they commonly develop around the cheeks and eye area. The six types of milia are:
- Neonatal milia
- Primary milia
- Secondary (traumatic) milia
- Juvenile milia
- Milia en plaque
- Multiple eruptive milia
4 Ways to Treat and Get Rid of Milia
Neonatal milia don’t require treatment because they can go away on their own. Milia in adults can last longer on the skin, but they don’t pose any health risks. They usually go away in a few weeks or months.
However, if a person is bothered by itchiness or by how milia look, there are some ways to treat them:
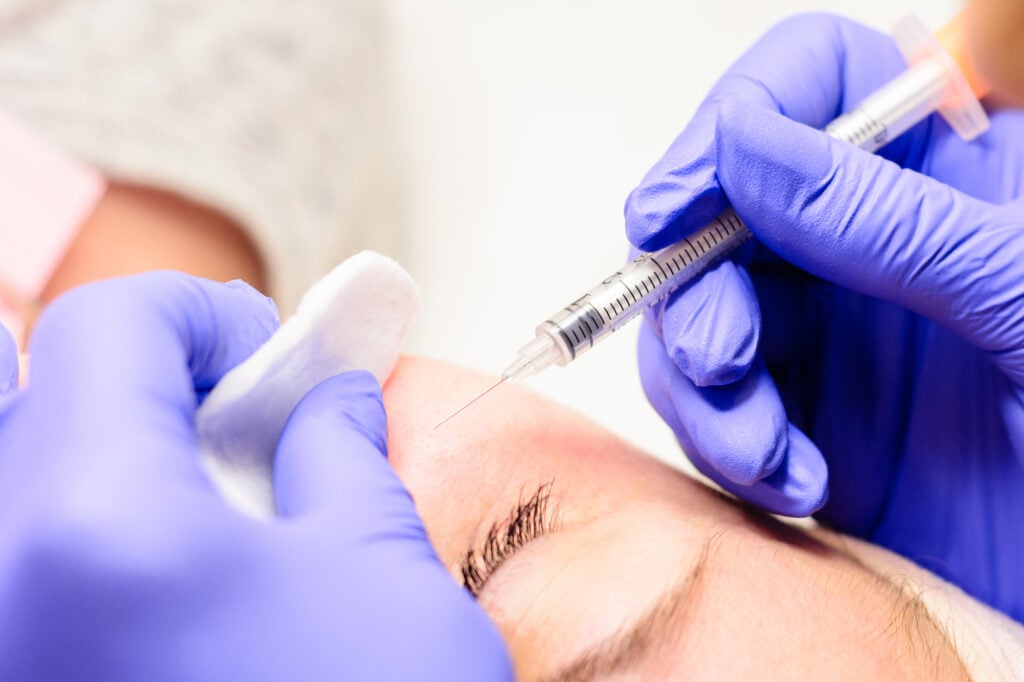
1. Manual Extractions by a Dermatologist (Best Option)
The most common form of extraction by a dermatologist is called de-roofing.10 Doctors will use a sterile needle to prick the bump and release the trapped keratin inside.
Doctors can also perform curettage or cryotherapy. Curettage involves scraping off milia and sealing the skin with a hot wire. Cryotherapy requires freezing off the bumps with liquid nitrogen.
Other procedures include:
- Dermabrasion
- Prescription medication
- Laser treatments
2. Topical Retinoid Creams
Topical retinoid creams are vitamin A-based medications and are popular for their anti-aging benefits. They are commonly used as an acne treatment, but some doctors prescribe them for people with milia.
Retinoids speed up the skin's turnover process and encourage the body to remove excess or dead cells in the outer skin layer, making it easier to extract milia. However, it does have the following side effects:
- Dryness
- Irritation
- Sun sensitivity
Because of these side effects, doctors don’t recommend this cream for people with dry or sensitive skin. Some over-the-counter (OTC) products are less irritating and weaker than prescription creams.
Studies show that it can take 3 to 6 months of regular use before noticeable skin improvements occur. The best results can take 6 to 12 months.5
3. Exfoliating Products (Salicylic/Glycolic Acid)
Using exfoliating products can help regulate skin cell turnover. It’s a great way to prevent more milia from forming because it ensures excess keratin flakes don’t build up.
Dermatologists recommend using chemical exfoliating products because they are more gentle than physical scrubs. They reduce the risk of irritation and redness around the affected area while removing dirt and dead skin cells.
The two exfoliants are beta hydroxy acids (BHA) and alpha hydroxy acids (AHA).
Some commonly used forms of BHAs include:
- Salicylic acid
- Willow extract
- Beta hydroxybutanoic acid
- Tropic acid
- Trethocanic acid
- Salicylate
- Sodium salicylate
Commonly used forms of AHAs include:
- Glycolic acid
- Lactic acid
- Citric acid
- Hydroxycaprylic acid
- Hydroxycapric acid
4. Wear Sunscreen
Wearing sunscreen is one of the most important home remedies for milia. Sun exposure and damage can cause secondary milia. It can also lead to clogged pores, which results in milia formation.
Using chemical exfoliants can also make the skin increasingly sensitive to the sun. Any milia treatment that involves chemical exfoliants needs to be accompanied by sunscreen.
Studies from the FDA show that after 4 weeks of AHA application, people’s sun sensitivity increased by 18%. They also showed that this sensitivity is reversible and does not last long once people stop using AHA products.1
Milia Symptoms
Depending on the type of milia, you may experience itchiness. Other symptoms of milia include:
- White or yellow bumps on your skin
- Appears on a raised patch of skin
- Bumps that appear in groups or clusters
- Bumps that don’t cause pain or discomfort
When Does a Milia Appear?
A milia appears at different stages of your life. Neonatal milia are seen in babies after birth and commonly occur around the nose. However, it’s possible to find some on the scalp, cheeks, and inside the mouth.
Primary and secondary milia can occur in both children and adults. On the other hand, Juvenile milia are cysts from an inherited condition. These may appear at birth or show up later in life.
Milia en plaque is a rare type that occurs around the ears, on the eyelids, or around the cheek and jaw area. They’re most common in middle-aged women.
Multiple eruptive milia occur in large patches over a period of weeks or months. They’re common around the face, upper arms, and torso. Similar to milia en plaque, this type is rare.
What Causes Milia?
Researchers haven’t determined the exact cause of milia. Primary milia can occur spontaneously on otherwise normal skin.
Experts believe milia form during the regeneration process in the sebaceous root of vellus hairs. These thin, barely noticeable hairs grow on the body during childhood. When the skin doesn’t turn over fast enough, a build-up of keratin forms, causing tiny bumps.
Secondary milia can develop after some form of damage or injury. Doctors believe damaged sweat glands are the underlying cause. They can also occur after applying corticosteroid creams to the skin.
Secondary milia can also occur from traumatic stimuli, which include:
- Dermabrasion
- Radiotherapy
- Second-degree burns
- Autologous skin grafts (for burns)
- Allergic contact dermatitis
- Prolonged topical steroid use
- Anti-inflammatory drug therapy
- Skin infections
Are Milia Harmful?
Milia are benign cysts that don’t pose a significant health risk. Health professionals commonly treat them as cosmetic issues.
In most cases, milia don’t have symptoms other than white bumps on the skin. However, if you have secondary milia, it’s possible to experience:
- Itchiness
- Irritation
- Swelling
Are AHA Exfoliants Safe to Use?
According to the Food and Drug Administration (FDA), AHAs are safe if certain conditions are met.1 These include:
- A concentration of 10% or less
- A pH of 3.5 or more
- Protects the skin from increased sun sensitivity
- Product packaging informs consumers to use daily sun protection
It’s also important to remember that exfoliant products meant to treat adult skin can harm newborn skin.
Don’t Remove Milia at Home
Dermatologists advise against extracting milia at home. Picking or squeezing the bumps can traumatize the skin and cause scarring.
Additional trauma to the skin can result in secondary milia, causing the condition to worsen. This makes it look like the bumps are spreading.
It’s normal for adult milia to go away for a few weeks or months. It’s best to consult a doctor for a professional procedure, such as extraction. A doctor can safely extract the bumps and ensure the skin doesn’t incur more damage.
Can You Prevent Milia?
There is no way to prevent neonatal milia because it spontaneously occurs as the baby is born. Parents can wash the baby’s face thrice weekly with warm water and gentle soap.
Parents should use patting motions to dry the skin afterward. Avoid using lotions or oils meant for adults on a baby’s skin. These can clog pores and cause more milia to develop.
Adults can create a proper skincare routine involving:
- Cleansing
- Exfoliating
- Sun protection
Dermatologists recommend using hypoallergenic products only to reduce the risk of irritation and the formation of secondary milia.
Summary
Milia are benign cysts that look like white bumps on the skin. They’re around 1 to 2 mm in diameter and commonly occur around the eye and cheek area.
Milia can occur spontaneously in newborns, children, and adults. They can also develop due to damage or trauma to the skin. They typically go away on their own.
Milia does not pose a significant risk to your health, and doctors generally consider it a cosmetic issue. Avoid picking or squeezing the bumps because doing so can damage the skin or cause more milia to form. See a doctor if you want them extracted.



