Double or blurry vision can be alarming, especially when your eyes suddenly won’t move as they should. These are concerning symptoms, and they can indicate ophthalmoplegia.
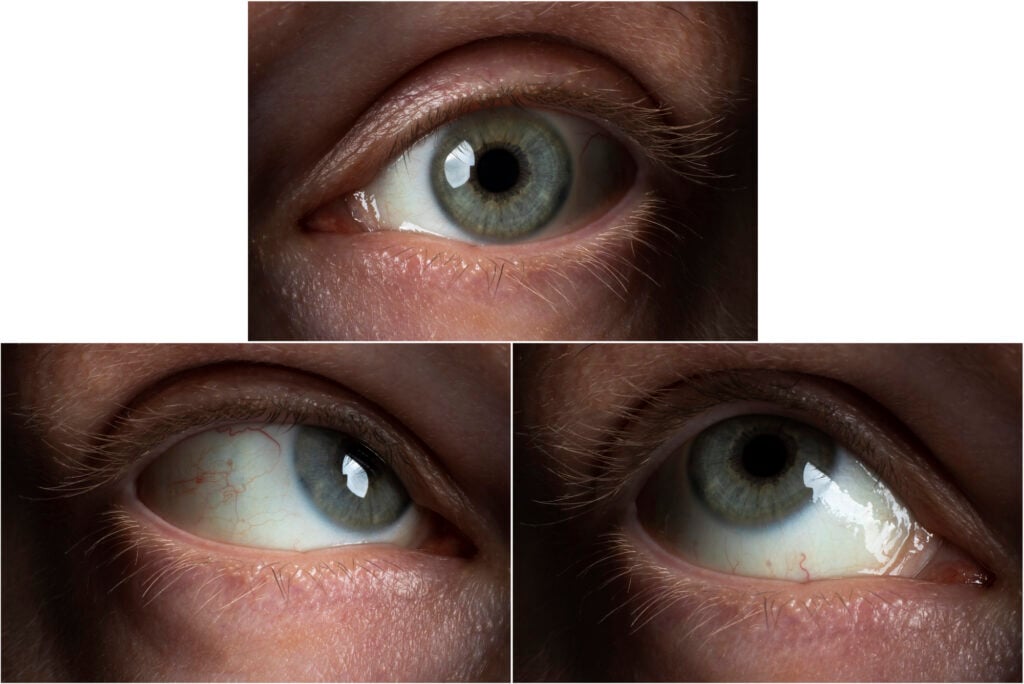
Ophthalmoplegia, or eye muscle weakness, can lead to various vision problems and requires medical treatment. This article will discuss the different types of ophthalmoplegia, its causes, and treatment.
What is Ophthalmoplegia?
Ophthalmoplegia refers to the weakness or paralysis of the eye muscles. The condition can affect one or more of the six muscles that keep the eye in place and control its movement.
Ophthalmoplegia can lead to eye movement abnormalities, and over time, the degree of your muscle control may decrease. If you experience the following, it is essential to contact your ophthalmologist:
- Blurred vision
- Double vision
- ‘Floaters’ in your vision
- A sudden headache
- Dizziness
What Are the Symptoms of Ophthalmoplegia?
People affected by ophthalmoplegia may experience the following:
- Double or blurred vision
- Inability to position the eyes in sync
- A challenging time moving both eyes in every direction
- Drooping eyelids (known as ptosis)
If ophthalmoplegia is linked to a systemic disorder, other symptoms may include problems with swallowing and general muscle weakness.
What are the Types of Ophthalmoplegia
Ophthalmoplegia cases may be split into two main groups: internal and external ophthalmoplegia. However, you should be aware of other types of ophthalmoplegia.
These include:
Internal Ophthalmoplegia
Internal ophthalmoplegia refers to paralysis or weakness in one of three internal muscles that help the eye focus and control pupil size.
This type of ophthalmoplegia may affect any of the following three internal muscles of the eye:
- Ciliary muscle. A ring of muscle that affects the shape of the lens. This enables the eye to focus on nearby or faraway objects.
- Dilator pupillae. A muscle that enlarges the size of the pupil to let in more light.
- Sphincter pupillae. A muscle that shrinks the size of the pupil to allow in less light.
External Ophthalmoplegia
External ophthalmoplegia is a weakness or paralysis in one of six muscles that work together to create eye movements. These muscles enable the eye to move up, down, side to side, and roll in a circle.
This type of ophthalmoplegia may affect any of the following six extraocular muscles:
- Superior rectus. A muscle fixed to the top of the eye that moves the eye upward.
- Inferior rectus. A muscle attached to the base of the eye that moves it downward.
- Medial rectus. A muscle fixed to the inside of the eye that moves it toward the nose.
- Lateral rectus. A muscle attached to the exterior of the eye that moves it toward the ear.
- Superior oblique. A muscle that rotates the eye downward and inward.
- Inferior oblique. A muscle that rotates the eye upward and outward.
Chronic Progressive External Ophthalmoplegia
A genetic mutation causes chronic progressive external ophthalmoplegia (CPEO). This type of ophthalmoplegia may affect one eye (unilateral) or both eyes (bilateral).
Those with CPEO may experience:
- Weakness in the eyelids
- Ptosis
- Problems swallowing (dysphagia)
- General weakness in the leg, arm, or neck muscles, especially following exercise
CPEO may result from different gene mutations. Inheritance patterns differ based on those mutations. In some cases, CPEO may develop as part of another condition.
For example, CPEO may occur with two neuromuscular disorders, such as ataxia neuropathy spectrum or Kearns-Sayre syndrome. Patients with either may experience other symptoms associated with those conditions.
Internuclear Ophthalmoplegia
Internuclear ophthalmoplegia results from a lesion in the brain’s medial longitudinal fasciculus (MLF). The MLF is a fiber tract in the brain that transfers information between the brain and the eyes.
The data transmitted by the MLF helps muscles to order eye movements. With internuclear ophthalmoplegia, the affected eye fails to adduct toward the nose, while the opposite eye abducts with nystagmus toward the ear.
The divergence of the eyes during internuclear ophthalmoplegia leads to horizontal diplopia. If the right eye is affected, the individual will have double vision when looking to the left.
This type of ophthalmoplegia may develop in one eye (unilateral internuclear ophthalmoplegia) or both eyes (bilateral internuclear ophthalmoplegia).
Supranuclear Ophthalmoplegia
Most people with supranuclear ophthalmoplegia suffer from progressive supranuclear palsy (PSP). PSP is a rare brain condition that leads to muscle weakness, walking issues, and other symptoms.
The term supranuclear refers to the affected brain area, which is an area above the nuclei. This type of ophthalmoplegia may also be called progressive supranuclear ophthalmoplegia. This means the disease worsens over time, and there is no cure.
What Causes Ophthalmoplegia?
Ophthalmoplegia can be congenital, which means present at birth, or it can develop later in life. The condition is typically caused by a disruption of the messages transferred from the brain to the eyes.
Internuclear ophthalmoplegia typically results from multiple sclerosis, infarction, or trauma. Meanwhile, chronic progressive external ophthalmoplegia is caused by genetic mutations and may be associated with underlying conditions, such as Kearns-Sayre syndrome.
Other common causes of Ophthalmoplegia include:
- Migraines
- Thyroid disease
- Stroke
- Brain injury
- Brain tumor
- Infection
What Are the Risk Factors of Ophthalmoplegia?
Ophthalmoplegia is slightly more common in people with diabetes. Older adults with long-standing type 2 diabetes (especially those with additional vascular risk factors) face an elevated risk of microvascular cranial-nerve palsies that manifest as ophthalmoplegia.
People with conditions that change their muscle control, like multiple sclerosis or Graves’ disease, are also more at risk than others.
Several vascular risk factors (such as smoking, hypertension, and poor glycemic control) can heighten the likelihood of ophthalmoplegia. Maintaining a healthy vascular system by following healthy lifestyle practices will reduce your risk of stroke and associated vision problems.
How is Ophthalmoplegia Treated?
Treatment for ophthalmoplegia depends on the condition’s type, symptoms, and underlying cause. Children born with ophthalmoplegia usually learn to compensate and may not be aware of their vision issues.
On the other hand, adults may receive special glasses or wear an eye patch to assist with double vision and help achieve normal vision. In some cases, treatments for migraines can result in improved outcomes for individuals with ophthalmoplegia.
Effective treatment of ophthalmoplegia targets the root cause and eases symptoms like double vision:
Steroids and immune therapy. Used for inflammation-related causes like thyroid eye disease or myasthenia gravis.
Surgical correction. Effective for stable eye misalignments after nerve palsies or trauma.
Botulinum toxin injections. Temporarily weaken overactive muscles, helping restore alignment.
Emerging therapies. Teprotumumab for thyroid eye disease and genetic research on POLG-related disorders hold promise for improved outcomes.
Prisms in glasses. Correct mild to moderate double vision quickly.
Special lenses: Occlusion foils blur one eye slightly, easing strain and discomfort.
Can You Prevent Ophthalmoplegia?
Ophthalmoplegia is usually a symptom of another syndrome or disease. However, regular visits to the eye doctor may help with early detection.
Even if you have normal vision, you should visit an eye specialist every two years. The eye possesses delicate muscles that rely on a healthy nervous and vascular system to function correctly.
People who have isolated ophthalmoplegia usually have a standard life expectancy. However, the underlying cause of the condition affects the overall prognosis.
Genetic and mitochondrial diseases, genetic syndromes, or a history of vascular disease or stroke can affect someone’s outlook significantly. It is essential to discover, address, and treat the underlying cause of your ophthalmoplegia for the best outcome.
How Do Eye Movement Pathways Break Down?
Your eye movements depend on a complex system involving nerves, brain structures, and extraocular muscles. Problems arise when these components fail:
- Cranial nerves. The third (oculomotor), fourth (trochlear), and sixth (abducens) cranial nerves directly control eye muscles. Damage to these nerves (nerve palsy) often leads to specific eye movement problems and double vision.
- Extraocular muscles. These muscles are highly specialized and vulnerable to mitochondrial disorders like Kearns-Sayre syndrome, causing chronic progressive external ophthalmoplegia.
- The medial longitudinal fasciculus (MLF). Damage here results in internuclear ophthalmoplegia, causing impaired inward eye movement.
- Brainstem lesions. Conditions like the one-and-a-half syndrome, caused by pontine lesions, produce complex patterns of horizontal gaze paralysis.
Why Do Certain Sites Fail?
Certain locations are particularly prone to dysfunction:
- Cranial nerve length. The sixth nerve has the longest intracranial course, making it vulnerable to increased pressure.
- Mitochondrial vulnerability. Extraocular muscles require constant energy, making mitochondrial diseases particularly debilitating (e.g., Kearns-Sayre syndrome).
- Vascular sensitivity. Cranial nerves often suffer ischemic injury from diabetes and hypertension, especially the third and sixth nerves.
- Pathway complexity. The MLF pathway's intricate connections make it vulnerable to small brainstem lesions, causing internuclear ophthalmoplegia.
Find Help for Ophthalmoplegia
Ophthalmoplegia needs monitoring and evaluation. To find specialized care and ensure optimal vision health, schedule a comprehensive eye exam with an experienced ophthalmologist.
Find an Eye Doctor near you through the American Academy of Ophthalmology (AAO).



